Hydration and Cognition in the General Population
Published
October 2020
Author
Matthew Wittbrodt; Kelly Barnes, MS, CPT

KEY POINTS:
- Individuals are not meeting their daily fluid requirements and therefore may be at risk for hypohydration.
- Hypohydration of 1% body mass loss or greater has been observed to impair cognition—mental processes required to perceive, process and produce information—which are required to accomplish everyday tasks.
- Children are at risk for hypohydration due to insufficient accessibility of water during the school day. Drinking water appears to improve cognitive performance in tasks required for optimal academic performance.
- Adults can achieve 1% of body mass loss or more with prolonged unintentional fluid restriction. This level of hypohydration may impair executive functioning and performance on functional tests such as driving.
- Older adults are at risk for hypohydration due to various factors including a muted thirst response and, if non-ambulatory, a risk of diminished water intake. While cognitive responses following acute hypohydration have not been robustly studied, hospital observation studies suggest water deficits can result in severe mental conditions such as acute confusion and delirium.
- Because thirst may act as a bottleneck for cognitive performance, effective countermeasures should revolve around diminishing thirst or, in the case of older adults, programmed drinking.
INTRODUCTION
Hydration is essential for life, and improper hydration (hypo- and hyper-) can elicit adverse physiological consequences. While the physical performance implications of hypohydration (i.e., under-hydrated) have been extensively reviewed (Cheuvront & Kenefick, 2014), the potential effects on cognitive and perceptual responses are less clear. Unlike aerobic exercise performance tests (e.g., time trial, time to exhaustion), which are more impaired in warm or hot environments with hypohydration due to greater cardiovascular strain and high skin temperature (Sawka et al., 1992), the neural constructs explaining cognitive decline are limited, in part, due to the complexity of brain circuitry and its relationship to monitoring the physiological state of the body. As such, no mechanism ascribing mental impairments to body water deficits exists. The responsible mechanism(s) also likely changes across the lifespan, as the developing and aging brain have different neural activations and/or alternative strategies to complete a given task. Within this Sports Science Exchange article, a brief description of cognitive function will be presented along with a brief overview of current state of the literature as it relates to hypohydration, cognitive performance, and children, adults and older adults. Finally, actionable items to maintain cognitive performance through improved hydration will be discussed.
Defining Fluid Requirements
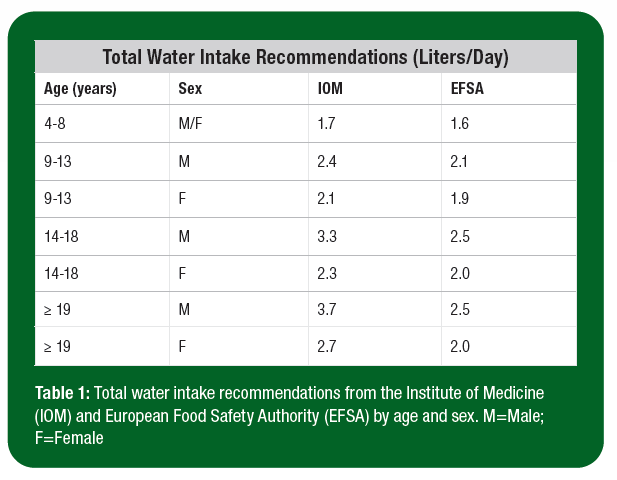
The consensus on fluid intake requirements from the Institute of Medicine (IOM, 2004) and the European Food Safety Authority (EFSA Panel on Dietetic Products, Nutrition & Allergies, 2010) are listed in Table 1. The fluid intake requirements are scientifically derived to understand the adequate intake of water required to prevent the adverse effects of dehydration (IOM, 2004). As such, factors such as health status, protein and salt intake, physical activity, and climate may contribute to large variability in water intake requirements at the individual level (IOM, 2004). A recent analysis of the 2011-2016 NHANES data found 60% of the population does not meet the IOM guidelines (Vieux et al., 2020), supporting early lab-based evidence that individuals are at risk for mild hypohydration even with adequate access to fluid, termed “voluntary dehydration” (Greenleaf & Sargent, 1965).
Defining Cognition
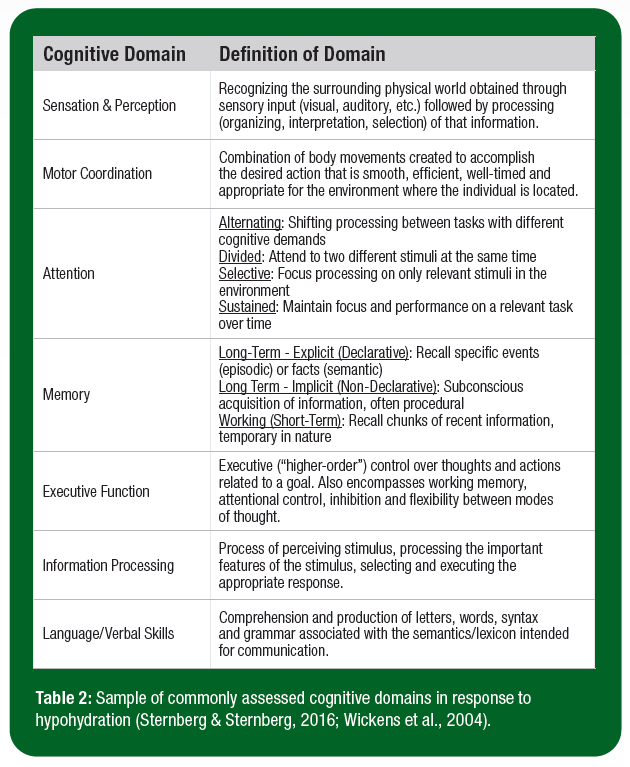
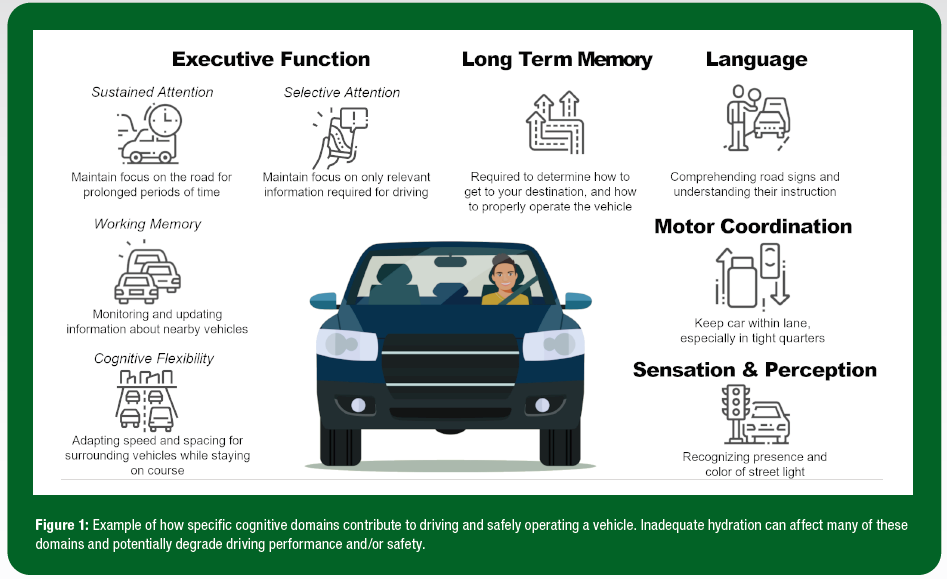
Cognitive psychology refers to the study of the structures, representations, and processes of the mind that take in, transform, and use information (Sternberg & Sternberg, 2016). For example, if asked to raise your hand when your name is called in a classroom, at each name spoken you are perceiving the auditory vocalization, recognizing the word as a name, accessing the knowledge of your name, deciding whether that name is yours, deciding whether you will raise your hand, and the controlling of your hand (should it be raised?). To assess cognitive performance, scientists have developed tests that stress specific aspects of cognitive processing. For example, a long-term memory task requires participants to listen to a paragraph and recall information about that paragraph 20-30 min later. In this task, aspects of cognitive processing beyond memory are minimized (i.e., the task should be easily heard, will not require a complex motor response) to isolate neural areas and processing related to memory. Quantifiable outcome measures such as accuracy or reaction time (i.e., speed of response) then provide objective measurements of performance. Ultimately, these tasks are important in facilitating our understanding of how hypohydration may impact cognitive performance by providing insights into which aspects of cognitive processing are most affected with body water deficits. Table 2 presents a sample of commonly assessed cognitive domains in the hypohydration literature; the definitions offered here are designed for practical understanding by individuals without a robust knowledge of cognitive psychology. Figure 1 presents an example of how multiple cognitive domains are required to accomplish the complex task of driving.
CHILDREN
Children are at risk for hypohydration due to insufficient consumption of fluid with breakfast, barriers at school and reliance on adults for access to fluids. As a result, ~60% (range: 10-98%) of children, across 19 countries, were found to not meet the fluid intake guidelines (Suh & Kavouras, 2019). Supporting the lack of fluid with breakfast, reports found 62% of children aged 9-11 arrived at school hypohydrated (Bonnet et al., 2012). During the school day, which constitutes approximately half their waking hours, children consumed only 14% of their daily total fluid intake (Bottin et al., 2019). Factors contributing to low fluid consumption at school are numerous, but of primary concern is a lack of access to beverages and/or inadequate knowledge of school staff regarding benefits, such as maintaining cognitive performance, of adequate fluid intake (Molloy et al., 2008). School-based interventions also have mixed efficacy, as one study observed no effect of education on drinking behavior in children (5th -6th-grade students) although water intake increased due to increased accessibility (Drozdowska et al., 2020).
In general, children have been understudied with regard to how hypohydration can impact cognitive performance. Because brain development continues until adulthood, children may be more vulnerable to the acute effects of hypohydration compared to adults. One of the only intervention studies used exercise in the heat to elicit 1.6% body mass (BM) loss and found that performance, on an executive function task, was unchanged despite greater brain activity during the task (Kempton et al., 2011). The authors argued that these findings represent an inefficient brain, meaning a greater level of effort was required to maintain the same performance. Other observational studies have found hydrated children performed better on a cognitive test battery compared to dehydrated children, with the strongest benefits of hydration occurring during the working memory task (Bar-David et al., 2005).
There is also strong evidence that drinking water (250 – 1,000 mL) has acute benefits to cognitive performance in children. Many reports have suggested drinking water improves performance in memory tasks such as working memory (Benton & Burgess, 2009), and visual (semantic) memory (Edmonds & Burford, 2009), although some studies suggest there is no effect (Edmonds & Jeffes, 2009). Studies on attention are also mixed, with some studies finding benefits of drinking water on visual attention (Chard et al., 2019; Edmonds & Burford, 2009; Edmonds & Jeffes, 2009) but others not finding benefits during sustained attention tasks (Benton & Burgess, 2009). However, children who were provided 200 mL of water on three occasions were more attentive to their school work, suggesting a practical benefit of drinking water (Benton, 2011).
ADULTS
Adults who limit water intake over 24 h can lose ≥ 1% BM with greater losses elicited with exercise and/or heat exposure (Stachenfeld et al., 2018). A recent meta-analysis completed in adults who lost ≥ 1% BM as a result of exercise, exercise + heat stress, heat stress or fluid restriction (Wittbrodt & Millard-Stafford, 2018a) found that hypohydration resulted in, (1) a small but significant overall impairment in cognitive performance, (2) greater cognitive impairments in higher-order domains such as executive function and attention compared to simple reaction time-based tests, and (3) greater cognitive impairments with >2% BM loss. Specific to this review, healthy adults losing ≥ 1% BM via free-living conditions (i.e., restricting fluid intake) or with simple exercise (no heat stress), had small but significant decreases in overall cognitive performance. While the small effect is likely due, in part, to the large variability among studies (e.g., different cognitive testing or hypohydration protocols), individual reports have indicated that hypohydration resulting from fluid restriction and/or exercise without added heat stress can impair executive function and spatial problem solving (Stachenfeld et al., 2018), working memory (Patel et al., 2007) and driving simulator performance (Watson et al., 2015).
Of the studies that found cognitive decrements with hypohydration using fluid restriction, it appears that executive functions were most impacted. This has been shown both during highly complex occupational simulation studies such as driving (Watson et al., 2015) and flight simulation (Lindseth et al., 2013) along with executive function-specific tasks (Stachenfeld et al., 2018). The occupational tasks are an intriguing look into human cognitive capacity following hypohydration, as they model complex behavior; that is, how can hypohydrated individuals simultaneously process multiple stimuli requiring perception, decision, memory and motor coordination. Within the occupational-specific studies, a couple of findings are of note. First, during prolonged driving, mild hypohydration (1.1% BM loss) more than doubled the overall number of driving mistakes (e.g., braking too late, drifting out of lane; 47 vs. 101) (Watson et al., 2015). Second, significant differences between the hypohydration and hydration conditions occurred only after 30 min, suggesting greater errors were due, in part, to the prolonged nature of the task. Additionally, the study by Lindseth et al. (2013) observed >2x the number of errors in a flight simulator with 1-3% BM loss, indicating that even highly practiced tasks can be impaired by hypohydration. This is an important finding, as hypohydration appears to increase mental workload as observed in brain imaging studies (Kempton et al., 2011; Watson et al., 2015; Wittbrodt et al., 2018b), which contribute to cognitive impairments (Wickens, 2008). Training decreases both the perceived (i.e., how difficult was the task?) and measured (i.e., brain activation levels) workloads during a given task (Borghini et al., 2013), and therefore these findings indicate hypohydration-mediated task impairments can occur independent of task proficiency.
While occupational task simulations provide invaluable feedback in “real-world” scenarios, tasks assessing discrete cognitive domains provide insight into how specific aspects of information processing are impaired by hypohydration. For example, in an assessment of a variety of cognitive domains, only the executive function tasks were impaired by hypohydration resulting from 24 h of fluid restriction (Stachenfeld et al., 2018). One specific executive function task affected was a test of paired associative learning. For example, if provided a list of state-color pairs (e.g., Michigan-Blue, New Hampshire-Green), one version of the task would ask participants to respond with the correct color if provided the state name. These cognitive processes are involved in learning and formulating relationships between items, which impacts most aspects of daily life. The other test impaired by hypohydration, the Groton Maze Learning Task, requires subjects to learn a sequence of dots presented on a grid. This is a test of visuospatial executive function and suggests the ability to learn and remember visuospatial patterns is impaired by hypohydration (Papp et al., 2011). This finding is reinforced by subsequent studies observing impairments in golf-specific distance judgment with fluid restriction of 12 h (Smith et al., 2012).
However, not all studies observe cognitive impairments with fluid restriction. For example, in a sample of males and females undergoing 28 h of fluid restriction (2.6% BM loss), hypohydration did not impact overall cognitive performance on a multi-domain cognitive battery (Szinnai et al., 2005). Furthermore, brain activity was not impacted during a task of information processing, conflicting with other studies finding increased brain activity with hypohydration. Interestingly, sex differences were observed with hypohydration (Szinnai et al., 2005). In a serial addition and Stroop (working memory, executive function) tasks, females had a slowing of reaction time (impaired performance) whereas men had a faster reaction time (increased performance). Unfortunately, few other studies have examined sex differences in cognitive performance following a bout of fluid restriction.
In addition to the objective performance measures collected in cognitive batteries (e.g., reaction time, accuracy), there has been a concerted effort to quantify the subjective feelings of individuals while hypohydrated. Indeed, many studies have observed deteriorated changes in subjective and affective feeling, often labeled as “changes in mood,” following fluid restriction of as little as 12 h (Pross et al., 2013). Some researchers have suggested the perceptual changes with hypohydration may contribute to and/or explain degradations in cognitive performance. This relationship may be modality-specific; that is, during fluid restriction protocols, worsened feelings may occur as a function of time whereas exercising in the heat may elicit similar changes through increased core temperature and/or greater perceived effort. For example, Petri et al. (2006) measured cognitive and affective change every 3 h throughout a day of fluid restriction (500 g/24 h) and observed continual decreases in global cognition and increases in ratings of energy required to complete the cognitive assessment. Lastly, other studies have identified that hypohydration (≥ 1% BM loss) alters specific symptoms related to worsened self-appraisal such as feelings of headache, decreased alertness, difficulty concentrating and greater fatigue (Shirreffs et al., 2004).
Like research in children, drinking water may restore cognitive decline brought on by hypohydration. Seminal work in adults by Denton and colleagues (Denton et al., 1999; Egan et al., 2003) have provided evidence that water, either swallowed or not, can decrease activation within the anterior cingulate, the thirst center in the brain. Importantly, the particular area of the anterior cingulate affected by thirst is involved in emotional perception and cognition (Devinsky et al., 1995). Therefore, this region may be a “bottleneck” in the competition between resources required to manage the thirst sensation and accomplish cognitive processing. For example, Edmonds et al. (2013) found drinking 500 mL of water following an overnight fast improved cognitive performance compared to the non-drinking trial only in the individuals experiencing the greatest severity of thirst. Drinking small volumes of water (150 mL) eliciting a negligible impact on fluid regulation improved cognitive performance which was mediated, in part, by changes in thirst and osmolality (Benton et al., 2016). These studies indicate that the presence of thirst may impair cognitive performance and therefore correcting this sensation may have beneficial effects.
OLDER ADULTS
There is a distinct lack of evidence on whether hypohydration may uniquely impair cognitive functioning in older adults (> 60 y). There is reason to believe cognitive faculties in older adults are disproportionately affected by hypohydration, such as a greater risk for acute confusion and delirium, which can lead to increased duration and severity of hospital stays (Inouye, 2006; Warren et al., 1994). Specifically, acute confusion is a mental condition consisting of increased irritability, distracted thinking and memory impairments, which have severe functional implications (Mentes & Buckwalter, 1997). Furthermore, older adults are at greater risk for hypohydration given several factors outlined previously (Kenney & Chiu, 2001; Lavizzo-Mourey, 1987; Spangler et al., 1984) including, (1) decreased concentration capacity of the kidney, (2) decreased efficacy of arginine vasopressin receptors in the kidney, (3) lower total body water due to reduced muscle mass (by ∼8%), (4) a muted thirst response to both hypovolemia and hypertonicity, (5) potential for diminished water intake if non-ambulatory, (6) prescription medications (e.g., loop diuretics) which alter water balance, and (7) taste preferences in beverages. These factors, in combination with other variables such as a greater risk for acute illness, infections and fever, are likely why community-based studies in older adults find an increased rate of hypohydration (Suhr et al., 2004).
With aging, it is difficult to understand the independent effects of hypohydration on cognitive performance without the context of the underlying neural systems. Older adults may present with age-related changes in the brain, such as decreased total brain volume and increased brain ventricle volumes, resulting from shrinking of the surrounding brain structures (Coffey et al., 1992). Along with the changes in brain structures (Carlson et al., 2008), aging presents other known neurobiological challenges, such as decreased concentration of the neurotransmitter acetylcholine (Sfera et al., 2016), which may partially explain the well-described decline in cognitive (Miquel et al., 2018) and motor (Buch et al., 2003) function.
To date, the limited studies in older adults present conflicting data regarding the effects of hypohydration on cognitive performance. In a sample of older adults (≥ 50 y) undergoing bowel preparation for a colonoscopy, no significant executive function decrements were observed despite a loss of 2% BM (Ackland et al., 2008). However, the nature of fluid loss is likely dissimilar to those elicited via sweat or lack of fluid ingestion. In a fluid restriction study, community-dwelling older (50 – 82 y) adults were observed to have slower psychomotor speed along with a modest decrease in working memory performance (Suhr et al., 2004). Furthermore, when attempting to model both psychomotor and working memory responses, the addition of hydration status significantly improved the model fit suggesting hydration status was related to the performance on the tasks (Suhr et al., 2004).
Additionally, observational studies have also found evidence of cognitive impairment with insufficient body water in older adults. When employing blood urea nitrogen to creatinine ratio as a proxy for hydration status (increased = greater hypohydration), an increased ratio was independently associated with a doubling of the risk to develop delirium (Inouye et al., 1993). In more free-living conditions, a post-hoc analysis of the 2011-2014 NHANES data found lower serum osmolarity (indicating improved hydration) was associated with better scores on the digit-symbol substitution test (attention, processing speed) in older-aged women but not men (Bethancourt et al., 2019).
While the current data is limited both in scope and volume, older adults are likely challenged in some capacity by the effects of hypohydration. The literature indicates hypohydration may be related to, at a minimum, worse executive processing and attention with more severe cases potentially manifesting in clinical conditions such as delirium (Inouye, 2006). How acute changes to hydration status (e.g., sweating during outdoor activity) alter the cognitive systems in older adults is currently unclear. Because older adults are already at risk for impairments in motor coordination (Buch et al., 2003), it is likely important to mitigate the potential influence of hypohydration, specifically concerning tasks observed to be at risk with body water deficits (e.g., driving) (Watson et al., 2015). Therefore, older adults (> 60 y) should be encouraged to maintain adequate hydration and, with respect to the diminished thirst sensation, may require cognitive strategies to consume adequate volumes of fluid (Table 1) such as filling a vessel with the daily allotment of water.
PRACTICAL APPLICATION AND SUMMARY
In summary, previous studies indicate fluid restriction can impair cognitive performance. Across the studies observing cognitive impairments with hypohydration, higher-order aspects of executive processing (executive function, attention, memory) appear more at risk than other tasks such as simple reaction time. The exact mechanism explaining these findings is unknown; however, the data in children and adults indicates quenching the thirst sensation may be an effective countermeasure and should be encouraged both at home and work/school. For children, accessibility to water during the school day and education of teachers/staff appear important to improving hydration status. In older adults, the consequences of hypohydration may be more severe (e.g., delirium, acute confusion) and, in combination with a less sensitive thirst sensation and other factors challenging hydration status, suggests other strategies, such as programmed drinking, may be beneficial.
Kelly Barnes is employed by the Gatorade Sports Science Institute, a division of PepsiCo, Inc. The views expressed are those of the authors and do not necessarily reflect the position or policy of PepsiCo, Inc.
References
Ackland, G.L., J. Harrington, P. Downie, J.W. Holding, D. Singh-Ranger, K. Griva, M.G. Mythen and S.P. Newman (2008). Dehydration induced by bowel preparation in older adults does not result in cognitive dysfunction. Anesth. Analg. 106:924-929.
Bar-David, Y., J. Urkin, and E. Kozminsky (2005). The effect of voluntary dehydration on cognitive functions of elementary school children. Acta Paediatr. 94:1667-1673.
Benton, D. (2011). Dehydration influences mood and cognition: a plausible hypothesis? Nutrients 3:555-573.
Benton, D., and N. Burgess (2009). The effect of the consumption of water on the memory and attention of children. Appetite 53:143-146.
Benton, D., K.T. Jenkins, H.T. Watkins, and H.A. Young (2016). Minor degree of hypohydration adversely influences cognition: a mediator analysis. Am. J. Clin. Nutr. 104:603-612.
Bethancourt, H.J., W.L. Kenney, D.M. Almeida, and A.Y. Rosinger (2019). Cognitive performance in relation to hydration status and water intake among older adults, NHANES 2011-2014. Eur. J. Nutr. E-pub ahead of print. PMID: 31776660.
Bonnet, F., E.M. Lepicard, L. Cathrin, C. Letellier, F. Constant, N. Hawili, and G. Friedlander (2012). French children start their school day with a hydration deficit. Ann. Nutr. Metab. 60:257-263.
Borghini, G., P. Arico, L. Astolfi, J. Toppi, F. Cincotti, D. Mattia, P. Cherubino, G. Vecchiato, A.G. Maglione, I. Graziani, and F. Babiloni (2013). Frontal EEG theta changes assess the training improvements of novices in flight simulation tasks. Conf. Proc. IEEE Eng. Med. Biol. Soc. 6619-6622.
Bottin, J.H., C. Morin, I. Guelinckx, and E.T. Perrier (2019). Hydration in children: What do we know and why does it matter? Ann. Nutr. Metab. 74(suppl 3):11-18.
Buch, E.R., S. Young, and J.L. Contreras-Vidal (2003). Visuomotor adaptation in normal aging. Learn. Mem. 10:55-63.
Carlson, N.E., M.M. Moore, A. Dame, D. Howieson, L.C. Silbert, J.F. Quinn, and J.A. Kaye (2008). Trajectories of brain loss in aging and the development of cognitive impairment. Neurology 70:828-833.
Chard, A.N.,V. Trinies, C.J. Edmonds, A. Sogore, and M.C. Freeman (2019). The impact of water consumption on hydration and cognition among schoolchildren: Methods and results from a crossover trial in rural Mali. PloS One 14:e0210568.
Cheuvront, S., and R. Kenefick (2014). Dehydration: physiology, assessment, and performance effects. Compr. Physiol. 4:257-285.
Coffey, C.E., W.E. Wilkinson, L. Parashos, S.A. Soady, R.J. Sullivan, L.J. Patterson, G.S. Figiel, M.C. Webb, C.E. Spritzer, and W.T. Djang (1992). Quantitative cerebral anatomy of the aging human brain A cross‐sectional study using magnetic resonance imaging. Neurology 42:527-527.
Denton, D., R. Shade, F. Zamarippa, G. Egan, J. Blair-West, M. McKinley, and P. Fox (1999). Correlation of regional cerebral blood flow and change of plasma sodium concentration during genesis and satiation of thirst. Proc. Natl. Acad. Sci. USA 96:2532-2537.
Devinsky, O., M.J. Morrell, and B.A. Vogt (1995). Contributions of anterior cingulate cortex to behaviour. Brain, 118:279-306.
Drozdowska, A., M. Falkenstein, G. Jendrusch, P. Platen, T. Luecke, M. Kersting, and K. Jansen (2020). Water consumption during a school day and children's short-term cognitive performance: The cognidrop randomized intervention trial. Nutrients 12:1297. E-pub ahead of print. PMID: 32370147.
Edmonds, C.J., and D. Burford (2009). Should children drink more water?: the effects of drinking water on cognition in children. Appetite 52:776-779.
Edmonds, C.J., and B. Jeffes (2009). Does having a drink help you think? 6-7-Year-old children show improvements in cognitive performance from baseline to test after having a drink of water. Appetite 53:469-472.
Edmonds, C.J., R. Crombie, and M.R. Gardner (2013). Subjective thirst moderates changes in speed of responding associated with water consumption. Front. Hum. Neurosci. 7:363.
EFSA Panel on Dietetic Products, Nutrition., & Allergies. (2010). Scientific opinion on dietary reference values for water. EFSA J. 8:1459.
Egan, G., T. Silk, F. Zamarripa, J. Williams, P. Federico, R. Cunnington, L. Carabott, J. Blair-West, R. Shade, M. McKinley, M. Farrell, J. Lancaster, G. Jackson, P. Fox, and D. Denton (2003). Neural correlates of the emergence of consciousness of thirst. Proc. Natl. Acad. Sci. USA 100:15241-15246.
Greenleaf, J.E., and F. Sargent (1965). Voluntary dehydration in man. J. Appl. Physiol. 20:719-724.
Inouye, S. (2006). Delirium in older persons. N. Eng. J. Med. 354:1157-1165.
Inouye, S.K., C.M. Viscoli, R.I. Horwitz, L.D. Hurst, and M.E. Tinetti (1993). A predictive model for delirium in hospitalized elderly medical patients based on admission characteristics. Ann. Intern. Med. 119: 474-481.
IOM. (2004). Dietary reference intakes for water, potassium, sodium, chloride, and sulfate. Washington, DC: National Academies Press.
Kempton, M., U. Ettinger, R. Foster, S. Williams, G. Calvert, A. Hampshire, F.O. Zelaya, R.L. O'Gorman, T. McMorris, A.M. Owen and M. Smith (2011). Dehydration affects brain structure and function in healthy adolescents. Hum. Brain Mapp. 32:71-79.
Kenney, W.L., and P. Chiu (2001). Influence of age on thirst and fluid intake. Med. Sci. Sports Exerc. 33:1524-1532.
Lavizzo-Mourey, R.J. (1987). Dehydration in the elderly: A short review. J. Nat. Med. Assoc. 79:1033-1038.
Lindseth, P.D., G.N. Lindseth, T.V. Petros, W.C. Jensen, and J. Caspers (2013). Effects of hydration on cognitive function of pilots. Mil. Med. 178:792-798.
Mentes, J., and K. Buckwalter (1997). Getting back to basics: Maintaining hydration to prevent acute confusion in frail elderly. J. Gerontol. Nurs. 23:48-51.
Miquel, S., C. Champ, J. Day, E. Aarts, B.A. Bahr, M. Bakker, D. Bánáti, V. Calabrese, T. Cederholm, J. Cryan, L. Dye, J.A, Farrimond, A. Korosi, S. Layé, S. Maudsley, D. Milenkovic, M.H. Mohajeri, J. Sijben, A. Solomon, J.P.E. Spencer, S. Thuret, W. Vanden Berghe, D. Vauzour, B. Vellas, J. Wesnes, P. Willatts, L. Wittenberg Rand, and L. Geurts (2018). Poor cognitive ageing: Vulnerabilities, mechanisms and the impact of nutritional interventions. Ageing Res. Rev. 42:40-55.
Molloy, C.J., J. Gandy, C. Cunningham, and G. Slattery (2008). An exploration of factors that influence the regular consumption of water by Irish primary school children. J. Hum. Nutr. Diet. 21:512-515.
Papp, K.V., P.J. Snyder, P. Maruff, J. Bartkowiak, and R.H. Pietrzak (2011). Detecting subtle changes in visuospatial executive function and learning in the amnestic variant of mild cognitive impairment. PLoS One 6:e21688.
Patel, A.V., J.P. Mihalik, A.J. Notebaert, K.M. Guskiewicz, and W.E. Prentice (2007). Neuropsychological performance, postural stability, and symptoms after dehydration. J. Ath. Train. 42:66-75.
Petri, N.M., N. Dropulić, and G. Kardum (2006). Effects of voluntary fluid intake deprivation on mental and psychomotor performance. Croat. Med. J. 47:855-861.
Pross, N., A. Demazières, N. Girard, R. Barnouin, F. Santoro, E. Chevillotte, A. Klein, and L. Le Bellego (2013). Influence of progressive fluid restriction on mood and physiological markers of dehydration in women. Br. J. Nutr. 109:313-321.
Sawka, M.N., A.J. Young, W.A. Latzka, P.D. Neufer, M.D. Quigley, and K.B. Pandolf (1992). Human tolerance to heat strain during exercise: influence of hydration. J. Appl. Physiol. 73:368-375.
Sfera, A., M. Cummings, and C. Osorio (2016). Dehydration and cognition in geriatrics: A hydromolecular hypothesis. Front. Mol. Biosci. 3:18.
Shirreffs, S.M., S.J. Merson, S.M. Fraser, and D.T. Archer (2004). The effects of fluid restriction on hydration status and subjective feelings in man. Br. J. Nutr. 91:951.
Smith, M.F., A.J. Newell, and M.R. Baker (2012). Effect of acute mild dehydration on cognitive-motor performance in golf. J. Strength Cond. Res. 26:3075-3080.
Spangler, P.F., T.R. Risley, and D.D. Bilyew (1984). The management of dehydration and incontinence in nonambulatory geriatric patients. J. Appl. Behav. Analysis 17:397-401.
Stachenfeld, N.S., C.A. Leone, E.S. Mitchell, E. Freese, and L. Harkness (2018). Water intake reverses dehydration associated impaired executive function in healthy young women. Physiol. Behav. 185:103-111.
Sternberg, R.J., and K. Sternberg (2016). Cognitive Psychology (7th ed.). Boston, MA: Cengage Learning.
Suh, H., and S.A. Kavouras (2019). Water intake and hydration state in children. Eur. J. Nutr. 58:475-496.
Suhr, J.A., J. Hall, S.M. Patterson, and R.T. Niinistö (2004). The relation of hydration status to cognitive performance in healthy older adults. Int. J. Psychophysiol. 53:121-125.
Szinnai, G., H. Schachinger, M.J. Arnaud, L. Linder, and U. Keller. (2005). Effect of water deprivation on cognitive-motor performance in healthy men and women. Am. J. Physiol. 289:R275-R280.
Vieux, F., M. Maillot, C.D. Rehm, P. Barrios, and A. Drewnowski (2020). Trends in tap and bottled water consumption among children and adults in the United States: analyses of NHANES 2011-16 data. Nutr. J. 19:10.
Warren, J.L., W.E. Bacon, T. Harris, A.M. McBean, D.J. Foley, and C. Phillips (1994). The burden and outcomes associated with dehydration among US elderly, 1991. Am. J. Public Health 84:1265-1269.
Watson, P., A. Whale, S.A. Mears, L.A. Reyner, and R.J. Maughan (2015). Mild hypohydration increases the frequency of driver errors during a prolonged, monotonous driving task. Physiol. Behav. 147:313-318.
Wickens, C.D. (2008). Multiple resources and mental workload. Hum. Fact. 50:449-455.
Wickens, C.D., S.E. Gordon, and Y. Liu (2004). An Introduction to Human Factors Engineering (2nd ed.). Upper Saddle River, New Jersey: Pearson Education.
Wittbrodt, M.T., and M. Millard-Stafford (2018a). Dehydration impairs cognitive performance: A meta-analysis. Med. Sci. Sports Exerc. 50:2360-2368.
Wittbrodt, M.T., M.N. Sawka, J.C. Mizelle, L.A. Wheaton, and M.L. Millard-Stafford (2018b). Exercise-heat stress with and without water replacement alters brain structures and impairs visuomotor performance. Physiol. Rep. 6:e13805.








