Practical Approaches to Nutrition for Female Athletes
Published
July 2021
Author
Bryan Holtzman; Kate Ackerman

KEY POINTS
- There are few nutritional recommendations developed specifically for female athletes, and most recommendations are based on studies of male athletes.
- The menstrual cycle may affect optimal nutrition strategies for performance, but menstrual cycles can be quite variable.
- Female athletes should first be concerned with attaining adequate energy availability, which ensures proper fueling for their exercise and basal physiologic and homeostatic functioning.
- Low energy availability can manifest as relative energy deficiency in sport (RED-S), a constellation of symptoms that can negatively affect numerous physiologic systems and athletic performance.
- Signs of nutritional deficiencies are reasons for medical evaluation by a sports medicine or primary care physician. Involving a sports dietitian can also be beneficial to the athlete.
INTRODUCTION
Signs of nutritional deficiencies are reasons for medical evaluation by a sports medicine or primary care physician. Involving a sports dietitian can also be beneficial to the athlete.
Athletes have been bombarded with nutritional advice from many sources. Social media has provided a platform for many people to promote specific nutritional programs purported to improve physique and performance, often without scientific basis or knowledge base. These programs can, in fact, be harmful to the athlete’s health or performance. Female athletes are particularly vulnerable to wayward nutrition advice, as up to 47% of female athletes have been shown to be at risk for caloric intake that is inadequate for their needs (Ackerman et al., 2019; Bratland-Sanda & Sundgot-Borgen, 2013). Unfortunately, sports research specific to women is lacking, leading to potentially incorrect application of findings in male studies to female athletes (Costello et al., 2014). In particular, the menstrual cycle is a uniquely female physiologic consideration that causes predictable yet inconsistent hormonal alterations in female athletes and contributes to the reticence about designing female-specific studies. For an in-depth discussion of these considerations, readers are directed to a recent review by Elliott-Sale and colleagues (2021). The upshot is that while women’s sport participation numbers rival that of men, the complexity and expense required to study women may contribute to the dearth of research.
This Sport Science Exchange article will review the nutritional recommendations for female athletes from a variety of perspectives. First, we will discuss the energetic requirements for athletes and the negative effects of failing to meet these requirements. Next, we will establish a model for meeting nutritional needs of increasing complexity and personalization for female athletes. Finally, we will provide some baseline recommendations for female athletes. This article aims to provide practical advice for athletes, coaches, physicians, and other members of the athlete entourage.
ENERGY AVAILABILITY
The most basic nutritional consideration for athletes is providing enough energy to power the workout, both on a day-to-day basis and longer-term perspective. The primary means of quantifying the achievement of this requirement are energy balance (EB) and energy availability (EA). Energy balance is simply the difference between kilocalories consumed in a day and kilocalories burned in a day (consisting of basal metabolic rate, thermic effect of food, and thermic effect of activity). While classically considered a static process, EB is actually mediated by a number of complex dynamic interactions (Holtzman & Ackerman, 2019; Thomas et al., 2016). Energy availability, on the other hand, is defined as the amount of energy that can be used for physiologic and homeostatic processes after accounting for exercise energy expenditure (EEE) and is the preferred measure of energy status for athletes (Thomas et al., 2016). Mathematically, EA is calculated as: . An EA of ~45 kcal·kg-1 FFM·day-1 is thought to be optimal for maintaining body size and mass, and allow for development of secondary sports skills (Loucks, 2013). An EA > 45 kcal·kg-1 FFM·day-1 allows for increased body mass, muscle hypertrophy, and carbohydrate loading, while an EA of 30–45 kcal·kg-1 FFM·day-1 will result in loss of body mass (Loucks, 2013). Classically, an EA < 30 kcal·kg-1 FFM·day-1 has been defined as “low EA” (Loucks et al., 1998), although the existence of this threshold has recently been called into question (Ackerman & Misra, 2018).
Relative energy deficiency in sport (RED-S)
While useful for sports science research, tracking EA for free-living athletes is challenging. Consequently, female athletes may not know they are suffering from inadequate EA until they begin to manifest symptoms of the energy insufficiency. The constellation of potential health and performance consequences that can arise secondary to low EA is known as relative energy deficiency in sport (RED-S) (Mountjoy et al., 2018). RED-S is an expansion of the well-described female athlete triad of low EA, reduced bone health, and menstrual dysfunction (De Souza et al., 2014) and posits that athletes can experience dysfunction in numerous physiologic systems owing to energy deficiency and that the symptomatology may be unique to each athlete. The potential health consequences and performance effects of RED-S are shown in Figure 1.
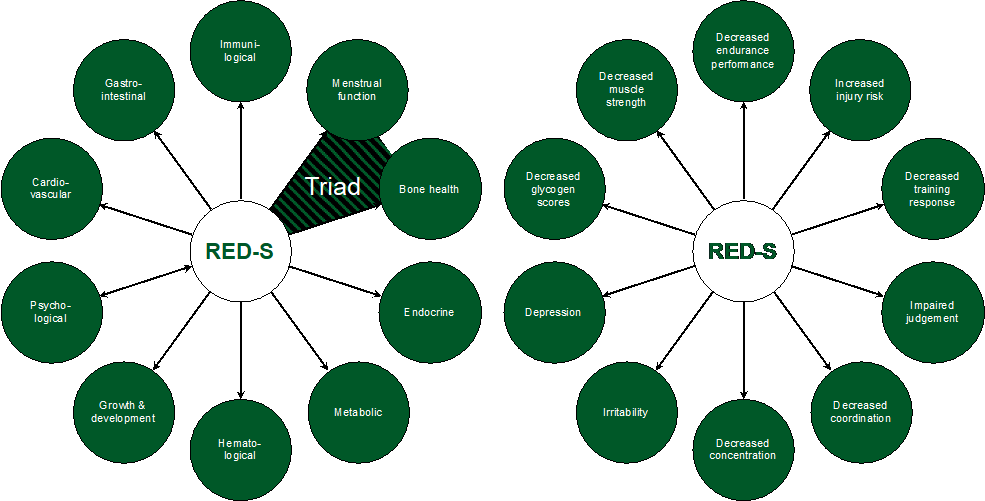
Figure 1. Health consequences (left) and performance effects (right) of RED-S. Adapted from Constantini (2002), with permission.
Unfortunately, many of the early symptoms of RED-S are vague and can be easily attributed to causes other than energy deficiency. Additionally, athletes who maintain a reasonable level of performance despite energy deficiency are likely operating at mildly reduced EA. Consequently, their illnesses may not fully present until many months or years of accumulation of energy deficit. It is thus paramount that all stakeholders in the athlete’s success maintain a high index of suspicion for RED-S when numerous, seemingly incongruous complaints arise. Potential manifestations of the health consequences are displayed in Table 1.
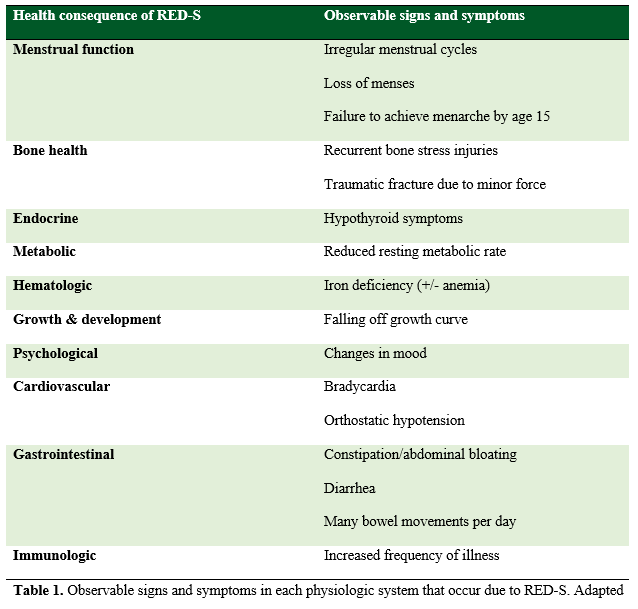
Table 1. Observable signs and symptoms in each physiologic system that occur due to RED-S. Adapted from Mountjoy et al. (2014; 2015; 2018) with permission.
Diagnosis and treatment of RED-S is beyond the scope of this review. If an athlete is suspected to have signs and symptoms of RED-S, she should be evaluated by a sports medicine physician. As is true in all medical fields, the best treatment of RED-S is prevention. An athlete at risk for energy deficiency would benefit from working with a sports dietitian to optimize her nutritional intake for her activity level. Unfortunately, there are many barriers to athletes seeing dietitians: cost, insurance coverage, and availability, to name a few. Athletes may find themselves at a loss for finding reasonable, fact-based strategies for fueling their athletic endeavors and passions.
NUTRITIONAL RECOMMENDATIONS FOR FEMALE ATHLETES
Establishing the Hierarchy of Nutritional Needs
To help bridge the gap between disparate information found on the internet and personalized expert advice, we propose a hierarchy of nutritional needs for female athletes (Figure 2). We recommend that each lower-level need be mostly satisfied sequentially prior to ascending to the next level in the hierarchy. We encourage female athletes to focus on laying a strong nutritional foundation prior to in-depth personalization.

Figure 2. Proposed hierarchy of nutritional needs and considerations for female athletes. When designing a nutritional plan, athletes should attempt to satisfy all lower-level needs before ascending the hierarchy.
Each higher level necessarily feeds back on lower levels. For example, an athlete may have satisfied her EA needs and ensured she is getting a reasonable distribution of macronutrients with adequate micronutrient intake. From there, she can time her intake of different components based on her exercise patterns for the day. An athlete who has yet to optimize her macro- and micronutrient intake, however, should focus on meeting those needs at baseline before making a nutrient timing plan. In some cases, increased athlete buy-in and adherence can be achieved by designing nutritional plans that focus on increasing caloric intake pre- and post-workout to improve overall EA. This is usually achieved under the guidance of a sports dietitian who is creating an individualized plan.
We propose that athletes adapt a gradual advancement of their nutritional plans much in the same way that training plans are graduated. As the athlete becomes more experienced with her nutrition (and training), she can ascend the hierarchy toward ultimate personalization. Flooding a less experienced athlete with many specific recommendations may overwhelm her and cause nonadherence, similar to how advancing a training plan too quickly can cause injury. For all athletes, the best nutrition plan is the one that she can follow.
The Menstrual Mediator
Recently, the menstrual cycle has become of particular interest as a mediator of exercise and nutrition effects. A normal menstrual cycle is characterized by rises and falls of estradiol and progesterone based on the phase of the cycle. Estradiol levels peak in the late-follicular phase and again in the mid-luteal phase, while progesterone peaks in the mid-luteal phase. The late-follicular estrogen peak induces hypothalamic release of gonadotropin-releasing hormone (GnRH) and subsequent peaks of luteinizing hormone (LH) and follicle-stimulating hormone (FSH). The “LH surge” causes ovulation. In the late-follicular phase, estradiol and progesterone levels wane following their mid-follicular peaks, and this reduction in hormone levels, particularly progesterone, causes menses.
Estrogen is an anabolic hormone and, of concern to athletes, it increases muscle strength and bone mineral density (BMD) (Baltgalvis et al., 2010; Lowe et al., 2010). Because of the monthly fluctuations in estrogen levels, matching the timing of training and nutrition with these hormonal changes has received attention as a way to improve performance. Furthermore, manipulation of the menstrual cycle with legal exogenous hormones (i.e., oral contraceptives) provides a theoretical opportunity for optimization. Many female athletes use oral contraceptives at baseline (Martin et al., 2018). Oral contraceptives may have a trivial negative effect on exercise performance, and there is no difference in exercise performance between the consumption and withdrawal phases of typical oral contraceptive use (Elliott-Sale et al., 2020). Use of oral contraceptives and other exogenous hormones, however, further complicates monitoring of natural hormonal fluctuations and research into menstrual mediation of athletic performance.
Little is known about the precise effects of the menstrual cycle on performance and how changing nutritional strategies dependent on menstrual phase can mitigate any nadirs. Poor study design, small sample sizes, and cost have all contributed to this lack of knowledge. Estrogen causes protein sparing, and studies at aerobic intensities have shown that women use more lipids and less carbohydrates and protein than men (Devries et al., 2006; Oosthuyse & Bosch, 2012; Wallis et al., 2006). Estrogen can also inhibit gluconeogenesis, and, in the mid-luteal phase (when estrogen levels are high), female athletes use less muscle glycogen during exercise compared with the follicular phase and when compared with male athletes. As such, increasing carbohydrate intake during the luteal phase may help to overcome this deficit (Devries et al., 2006; McNulty et al., 2020). Female athletes, however, are more prone to non-regular menstrual cycles (oligomenorrhea), absent menstrual cycles (amenorrhea), and defective menstrual cycles (e.g., anovulatory cycles, luteal phase defect) (Redman & Loucks, 2005). Because little is known about how performance changes during the menstrual cycle (McNulty et al., 2020), generating generalized nutritional advice is difficult. We recommend that exercising women ensure adequate caloric intake to have regular cycles and then use a personalized approach based on qualitative factors to fine-tune their nutritional plan to their cycles.
Macronutrients
Protein, carbohydrate, and fat are the three macronutrients consumed in the diet. Each plays a specific role in exercise. Protein is important for muscle anabolism and other anabolic processes. Carbohydrates are rapidly available and can be replenished during extended bouts of exercise. Fat is used to fuel aerobic exercise of long duration. Diversity in macronutrient intake will naturally endow diversity in micronutrient intake. The American College of Sports Medicine recommends that exercising women consume 1.2–2 g×kg-1×day-1 of protein (Thomas et al., 2016). However, higher progesterone levels may increase the protein requirement during the luteal phase due to higher rates of protein catabolism (Oosthuyse & Bosch, 2010).
Carbohydrate is the macronutrient of primary concern before, during, and after exercise. Unfortunately, most studies that serve as the foundations for carbohydrate intake strategies were conducted in male athletes (Rehrer et al., 2017). At exercise intensities > 50% maximal oxygen consumption (VO2max), rates of gluconeogenesis are higher in the follicular phase than in the luteal phase (Campbell et al., 2001; Zderic et al., 2001). Consequently, exercise performance may be impaired during the follicular phase, and this impairment can be mitigated by consuming a carbohydrate-rich snack 3 to 4 hours prior to exercise (Rehrer et al., 2017). Carbohydrate consumption during endurance exercise is dependent on duration: for sessions lasting 1–2.5 hr, 30–60 g/hr carbohydrate can improve performance, and for durations > 2.5 hr, some data suggest that consuming > 90 g/hr carbohydrate can improve performance (Thomas et al., 2016). Notably, carbohydrate recommendations during exercise are not weight-based. Following exercise, athletes are recommended to consume ≥ 1.2 g×kg-1×hr-1 carbohydrate for 4–6 hours. Alternatively, adding protein in a 4:1 carbohydrate:protein ratio can aid in recovery if the former carbohydrate intake recommendation cannot be met (Kerksick et al., 2017). Specific recovery strategies will in part be dictated by the timing of the next exercise session.
Pre-competition “carb loading”—increasing carbohydrate intake in the days prior to endurance competition—is a common nutritional strategy employed by athletes at all levels. Women oxidize more fat and less carbohydrate than men at the same relative exercise intensities, again confounding the interpretation and application of many studies that were primarily conducted in male athletes (Tarnopolsky, 2000). For events lasting < 90 min, dedicated carb loading is not necessary, and glycogen stores can be replenished with regular consumption of 7–10 g×kg-1×day-1 carbohydrate (Burke et al., 2011). When an athlete is competing in an event lasting ≥ 90 min, consuming 10–12 g×kg-1×day-1 carbohydrate for 36–48 hr before competition may improve performance (Burke et al., 2011; Thomas et al., 2016). Menstrual phase may affect intake strategies: consuming 8.4–9 g×kg-1×day-1 carbohydrate in the mid-follicular phase increases muscle glycogen levels but has not been shown to improve performance. Luteal loading has less of an effect or no effect on glycogen stores, and performance changes remain unclear (McLay et al., 2007; Walker et al., 2000). Whether these effects are present with oral contraceptive use is unknown.
Fat consumption recommendations have not been studied in relation to the menstrual cycle. Current recommendations suggest that athletes should consume at least 20% of their calories as fats (Thomas et al., 2016). Of note, vitamins A, D, E, and K are fat-soluble, and inadequate fat intake can result in insufficiency of these vitamins.
Micronutrients
Micronutrients include vitamins and minerals that are consumed in the diet and are necessary for cellular function. Low EA can cause micronutrient deficiencies. Female athletes are particularly prone to deficiencies in iron, calcium, and vitamin D, even with adequate EA. Recommendations for intake of these micronutrients are shown in Table 2.
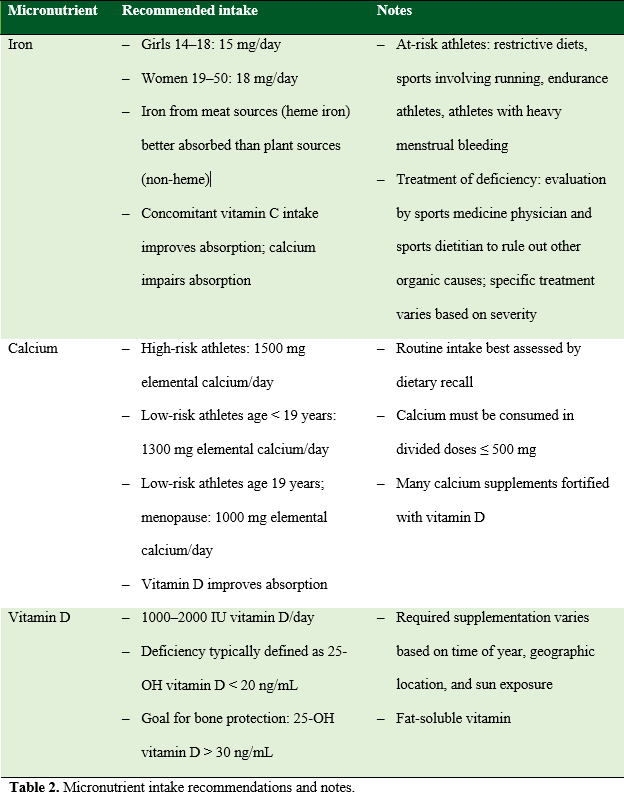
Table 2. Micronutrient intake recommendations and notes.
PRACTICAL APPLICATIONS
- Nutrition plans should advance from simple to complex as an athlete becomes more experienced.
- Consultation with a sports dietitian can identify nutritional deficiencies and improve plans.
- Adequate energy availability sets the foundation for athlete health and performance.
- Evidence for tailoring nutrition to menstrual cycle phase is in its infancy. For most athletes, altering nutrition based on qualitative factors (e.g., bloating) is sufficient until more is known.
CONCLUSIONS
As participation in female sports continues to rise worldwide, the lack of female athlete–specific recommendations and research into nutritional considerations of health and performance has become a focus of stakeholders in female athlete success. Many current recommendations are based on studies of male athletes, and these recommendations may not account for female physiology, such as the menstrual cycle, hormonal contraceptive use, injury risk factors, and body size and composition. Nevertheless, we have provided an overview of the current state of evidence for nutritional strategies and provided recommendations to promote health and performance of female athletes. The possible causes of nutritional deficiencies are broad, and any concerns or signs of deficiency should prompt a workup by a sports medicine or primary care physician.
The views expressed are those of the authors and do not necessarily reflect the position or policy of PepsiCo, Inc. The authors thank Rose K. Kelly for her primary research assistance.
References
Ackerman, K.E., B. Holtzman, K.M. Cooper, E.F. Flynn, G. Bruinvels, A.S. Tenforde, K.L. Popp, A.J. Simpkin, and A.L. Parziale (2019). Low energy availability surrogates correlate with health and performance consequences of Relative Energy Deficiency in Sport. Br. J. Sports Med. 53:628-633.
Ackerman, K.E., and M. Misra (2018). Amenorrhoea in adolescent female athletes. Lancet Child Adolescent Health 2:677-688.
Baltgalvis, K.A., S.M. Greising, G.L. Warren, and D.A. Lowe (2010). Estrogen regulates estrogen receptors and antioxidant gene expression in mouse skeletal muscle. PloS One 5:e10164.
Bratland-Sanda, S., and J. Sundgot-Borgen (2013). Eating disorders in athletes: overview of prevalence, risk factors and recommendations for prevention and treatment. Eur. J. Sport Sci. 13:499-508.
Burke, L.M., J.A. Hawley, S.H. Wong, and A.E. Jeukendrup (2011). Carbohydrates for training and competition. J. Sports Sci. 29(suppl 1):S17-S27.
Campbell, S.E., D.J. Angus, and M.A. Febbraio (2001). Glucose kinetics and exercise performance during phases of the menstrual cycle: effect of glucose ingestion. Am. J. Physiol. 281:E817-E825.
Constantini, N.W. (2002). Medical concerns of the dancer. Book of Abstracts. FIMS World Congress of Sports Medicine Budapest.
Costello, J.T., F. Bieuzen, and C.M. Bleakley (2014). Where are all the female participants in sports and exercise medicine research? Eur. J. Sport Sci. 14:847-851.
De Souza, M.J., A. Nattiv, E. Joy, M. Misra, N.I. Williams, R.J. Mallinson, J.C. Gibbs, M. Olmsted, M. Goolsby, G. Matheson, and P. Expert (2014). 2014 Female athlete triad coalition consensus statement on treatment and return to play of the female athlete triad. Br. J. Sports Med. 48:289.
Devries, M.C., M.J. Hamadeh, S.M. Phillips, and M.A. Tarnopolsky (2006). Menstrual cycle phase and sex influence muscle glycogen utilization and glucose turnover during moderate-intensity endurance exercise. Am. J. Physiol. 291:R1120-R1128.
Elliott-Sale, K.J., K.L. McNulty, P. Ansdell, S. Goodall, K.M. Hicks, K. Thomas, P.A. Swinton, and E. Dolan (2020). The effects of oral contraceptives on exercise performance in women: a systematic review and meta-analysis. Sports Med. 50:1785-1812.
Elliott-Sale, K.J., C.L. Minahan, X. de Jonge, K.E. Ackerman, S. Sipila, N.W. Constantini, C.M. Lebrun, and A.C. Hackney (2021). Methodological considerations for studies in sport and exercise science with women as participants: a working guide for standards of practice for research on women. Sports Med. 51:843-861.
Holtzman, B., and K.E. Ackerman (2019). Measurement, determinants, and implications of energy intake in athletes. Nutrients, 11:665.
Kerksick, C.M., S. Arent, B.J. Schoenfeld, J.R. Stout, B. Campbell, C.D. Wilborn, L. Taylor, D. Kalman, A.E. Smith-Ryan, R.B. Kreider, D. Willoughby, P.J. Arciero, T.A. VanDusseldorp, M.J. Ormsbee, R. Wildman, M. Greenwood, T.N. Ziegenfuss, A.A. Aragon, and J. Antonio (2017). International society of sports nutrition position stand: nutrient timing. J. Int. Soc. Sports Nutr. 14:33.
Loucks, A.B. (2013). Energy balance and energy availability. The Encyclopaedia of Sports Medicine: An IOC Medical Commission Publication, 19:72-87.
Loucks, A.B., M. Verdun, and E.M. Heath (1998). Low energy availability, not stress of exercise, alters LH pulsatility in exercising women. J. Appl. Physiol. 84:37-46.
Lowe, D.A., K.A. Baltgalvis, and S.M. Greising (2010). Mechanisms behind estrogen's beneficial effect on muscle strength in females. Exerc. Sport Sci. Rev. 38:61-67.
Martin, D., C. Sale, S.B. Cooper, and K.J. Elliott-Sale. (2018). Period prevalence and perceived side effects of hormonal contraceptive use and the menstrual cycle in elite athletes. Int. J. Sports Physiol. Perf. 13:926-932.
McLay, R.T., C.D. Thomson, S.M. Williams, and N.J. Rehrer (2007). Carbohydrate loading and female endurance athletes: effect of menstrual-cycle phase. Int. J. Sport Nutr. Exerc. Metab. 17:189-205.
McNulty, K.L., K.J. Elliott-Sale, E. Dolan, P.A. Swinton, P. Ansdell, S. Goodall, K. Thomas, and K.M. Hicks (2020). The effects of menstrual cycle phase on exercise performance in eumenorrheic women: a systematic review and meta-analysis. Sports Med. 50:1813-1827.
Mountjoy, M., J. Sundgot-Borgen, L. Burke, S. Carter, N. Constantini, C. Lebrun, N. Meyer, R. Sherman, K. Steffen, R. Budgett, and A. Ljungqvist (2014). The IOC consensus statement: beyond the Female Athlete Triad--Relative Energy Deficiency in Sport (RED-S). Br. J. Sports Med. 48:491-497.
Mountjoy, M., J. Sundgot-Borgen, L. Burke, S. Carter, N. Constantini, C. Lebrun, N. Meyer, R. Sherman, K. Steffen, R. Budgett, A. Ljungqvist, and K. Ackerman (2015). RED-S CAT. Relative Energy Deficiency in Sport (RED-S) Clinical Assessment Tool (CAT). Br. J. Sports Med. 49:421-423.
Mountjoy, M., J.K. Sundgot-Borgen, L.M. Burke, K.E. Ackerman, C. Blauwet, N. Constantini, C. Lebrun, B. Lundy, A.K. Melin, N.L. Meyer, R.T. Sherman, A.S. Tenforde, M.K. Torstveit, and R. Budgett (2018). IOC author consensus statement update 2018: Relative Energy Deficiency in Sport (RED-S). Br. J. Sports Med. 52:687-697.
Oosthuyse, T., and A.N. Bosch (2010). The effect of the menstrual cycle on exercise metabolism: implications for exercise performance in eumenorrhoeic women. Sports Med. 40:207-227.
Oosthuyse, T., and A.N. Bosch (2012). Oestrogen's regulation of fat metabolism during exercise and gender specific effects. Curr. Opin. Pharmacol. 12:363-371.
Redman, L.M., and A.B. Loucks (2005). Menstrual disorders in athletes. Sports Med. 35:747-755.
Rehrer, N.J., R.T. McLay-Cooke, and S.T Sims (2017). Nutritional strategies and sex hormone interactions in women. In: Sex Hormones, Exercise and Women. Springer, pp. 87-112.
Tarnopolsky, M.A. (2000). Gender differences in metabolism; nutrition and supplements. J. Sci. Med. Sport 3:287-298.
Thomas, D.T., K.A. Erdman, and L.M. Burke (2016). Position of the Academy of Nutrition and Dietetics, Dietitians of Canada, and the American College of Sports Medicine: Nutrition and Athletic Performance. J. Acad. Nutr. Dietet. 116:501-528.
Walker, J.L., G.J. Heigenhauser, E. Hultman, and L.L. Spriet (2000). Dietary carbohydrate, muscle glycogen content, and endurance performance in well-trained women. J. Appl. Physiol. 88:2151-2158.
Wallis, G.A., R. Dawson, J. Achten, J. Webber, and A.E. Jeukendrup (2006). Metabolic response to carbohydrate ingestion during exercise in males and females. Am. J. Physiol. 290:E708-715.
Zderic, T.W., A.R. Coggan, and B.C. Ruby (2001). Glucose kinetics and substrate oxidation during exercise in the follicular and luteal phases. J. Appl. Physiol. 90:447-453.








