A Sports Practitioner’s Perspective on the Return to Play During the Early Months of the COVID-19 Pandemic: Lessons Learned and Next Steps
Published
August 2021
Author
George T. Chiampas; Megan L. Chenworth; Eric Power; Abiye L. Ibiebele
Topics

Key Points:
- COVID-19, the disease caused by SARS-CoV-2, is a severe respiratory illness that has profound impact on health and presents unique challenges to the sporting community.
- It is important to establish preventative measures, such as masks, physical distancing, symptom monitoring, testing, and contact tracing along with clear, evidence-based guidelines for safe return to play after athletes have been exposed to and/or infected with COVID-19.
- Organizations must continue to implement scalable protocols for travel and use of athletic facilities, which allow for physical distancing and minimize risk of virus transmission, as well as distribution of vaccines as they become more widely available.
- Athletes recovering from COVID-19 should be monitored for cardiac and pulmonary complications after successful return to play, although these complications are rarer than initially thought.
- The use of an Incident Command Structure is one example of how organizations can successfully implement strategies to reduce transmission and enforce effective measures for return to play.
INTRODUCTION
The onset of the COVID-19 pandemic created new challenges and obstacles with regard to sports medicine. The discovery of this novel, highly transmissible disease, which carried potentially severe impacts on the health of the general population, had a significant effect on the sporting world. When COVID-19 was officially declared a pandemic by the World Health Organization (WHO) on March 11, 2020, a rapid, widespread shutdown of sports soon followed. This included cancellation or rescheduling for almost all professional and recreational sports organizations, as well as major events, such as the 2020 Summer Olympic Games in Tokyo. The novelty and reported severity of COVID-19 required a rapid response, and important decisions had to be made every day, even while new information emerged regarding transmissibility, at-risk populations, natural course of the illness, and medical management options.
While COVID-19 presented new challenges, the approach and tools that organizations and medical professionals needed to face these challenges were not new. Throughout the history of sport, there have been instances where external events, known and unknown, have presented health and safety risks to participants and spectators. Two high-profile instances in recent history include the Boston Marathon in 2013 and the Paris terror attacks during the France vs. Germany soccer match in 2015. These events were also unexpected, requiring swift mobilization and responses to address the medical needs of athletes, onlookers, and the community. Although events of this magnitude are uncommon, inclement weather incidents, natural disasters, or climate events such as extreme heat happen much more frequently and often lead to delays, rescheduling, and cancellations. An important necessity for all these scenarios, including the COVID-19 pandemic, is the adaption of a framework that is composed of a clear management structure that allows for efficient, effective communication and situational awareness to all stakeholders and participants in the face of rapidly changing information. This Sports Science Exchange article will provide a sports practitioner’s perspective on the return to play during the early months of the COVID-19 pandemic.
INCIDENT COMMAND
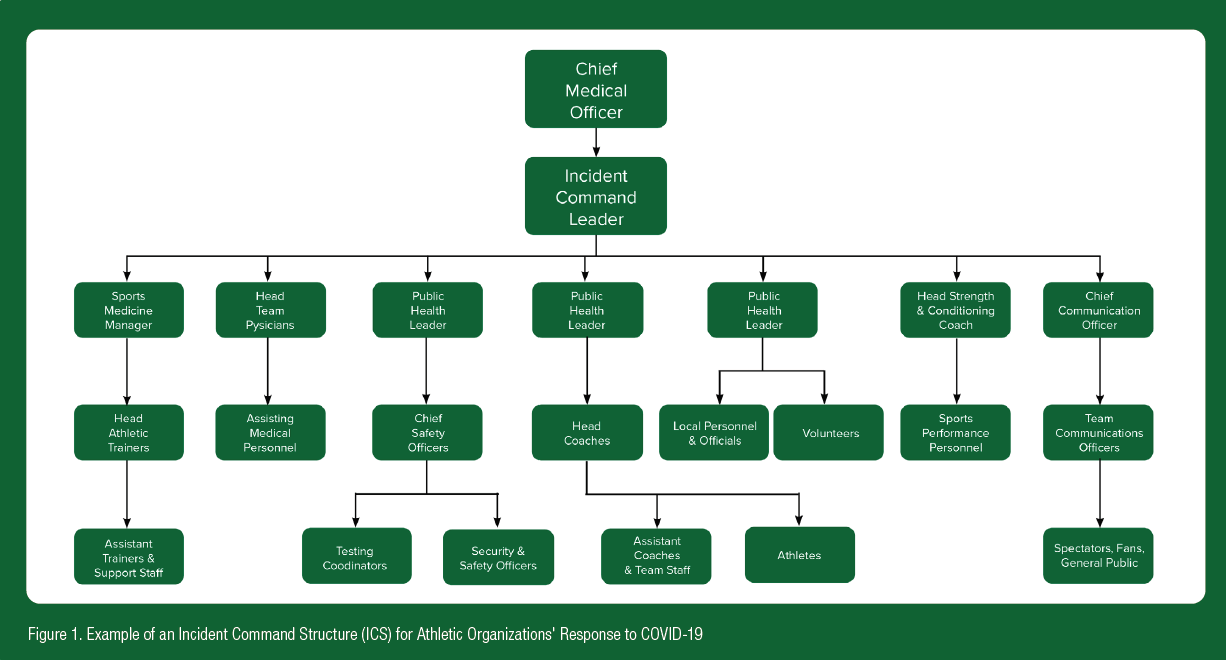
In 2001, the United States Department of Homeland Security developed the National Incident Management System (NIMS), which gives great insights into how to facilitate rapid communication and manage unexpected occurrences at high-profile events, such as those previously mentioned. The implementation of this system domestically has led to widespread use of an Incident Command Structure (ICS), which creates an organized system by which to address unique and spontaneous issues effectively and efficiently. An ICS is composed of a multidisciplinary team with clearly defined roles, often tailored to the specific needs of an incident (Figure 1). The team should be led by an incident commander, defined by the Federal Emergency Management Agency (FEMA) as the individual responsible for all incident activities, including the development of strategies and tactics and the ordering and release of resources (FEMA, 2021). The incident commander depends on the incident; in the sports and athletic arena, this should be someone who routinely operates as a critical decision maker in times of crisis. This is best carried out by a medical professional who consistently deals with making decisions quickly and in crises, such as emergency physicians. Other examples of important roles include public information officers, to facilitate communication with the target population, and safety officers, to mitigate risk and prioritize the safety of participants and staff (NIMS, 2017). Other roles are more specific to the situation, such as utilizing medical professionals with expertise in relevant fields as a trusted source to communicate information about COVID-19 to the public, as well as involving team physicians as resources to guide coaches, athletes, and other staff on safe return-to-play measures.
Just one example of the practical use of an ICS was the cancellation of the 2007 Chicago Marathon due to record high race day temperatures and humidity, which required police officers and volunteers to communicate vital information about the event to tens of thousands of participants accurately and in a timely manner. The ability to utilize an ICS, such as in this situation, involves not only effective implementation while facing the challenging situation, but also requires deliberate preparation in the months leading up to the event. Just a few examples of this preparation include: setting disaster plans, creating command structures, and recognition by planners that the event has the potential to be a “disaster,” in terms of number of individuals affected and the strain on local resources, if a worst-case scenario becomes reality.
COVID-19
All forms of mass gathering, including entertainment venues, public assemblies, and sporting events have faced unique challenges due to COVID-19. When first discovered during the outbreak in Wuhan, China, Li et al. (2020) described the COVID-19 virus as having significant human-to-human transmission, with each infected person, on average, spreading the virus to at least two other individuals. Initially, the method of transmission was thought to be through both respiratory droplets and direct contact. It is now known that the spread is primarily through respiratory droplets, with the potential for airborne transmission in certain situations, such as being indoors without adequate ventilation. This potential for airborne transmission creates the possibility of “super-spreader events” (Ways COVID-19 spreads, Centers for Disease Control and Prevention (CDC), 2020). Recent data from the WHO suggest the vast majority (80%) of people who contract COVID-19 recover without needing hospitalization, while about 15% become seriously ill (requiring supplemental oxygen), and 5% become critically ill (requiring intensive care) (WHO, 2020). Overall, mortality rates of those infected are estimated to be between 1.4% and 3.2% (Guan et al., 2020). Although severe disease and death are seen primarily in individuals over the age of 60 and those with medical comorbidities, there have also been deaths in young, healthy people. To put this in perspective, data from the CDC on influenza, another common respiratory virus, showed a 1.3% hospitalization rate and death rate between 0.029% and 0.065%, demonstrating the severity of COVID-19 (Estimated influenza illnesses, CDC, 2020).
IMPACT ON SPORT
The COVID-19 pandemic had a profound and rapid impact on the entire sporting world. On the same day the WHO officially declared COVID-19 a pandemic, the National Basketball Association (NBA) became the first domestic major professional sports organization in the United States to announce suspension of play due to the virus. This was followed just one day later by an announcement from the National Collegiate Athletic Association (NCAA) reporting the cancellation of its men’s and women’s basketball tournaments, as well as all remaining winter and spring championships (Osburn, 2020). Organizations at all levels of sport soon announced suspensions or cancellation of play. In situations like this, where multiple organizations with a wide disparity in available resources are trying to create a unified message, it is vital for information to be shared openly and for plans to be communicated quickly, between and within organizations. One way to avoid confusion among athletes, coaches, volunteers, and other stakeholders was to implement an ICS, or similar system, which many organizations already had in place. After the decision was made to shut down sport near universally, the community entered a different phase of planning to determine how to restart sports in a manner that kept everyone involved healthy and safe.
RETURN TO PLAY
Once organizations like the Olympic Games, the NCAA, and NBA made the decision to end seasons early and cancel championships, the focus shifted to ways in which the public and sports world could re-enter, and restart in a way that keeps our athletes, coaches, staff, and public safe. To do this, one first needed to expand the concept of team to include not only the athletes, but also the coaches, managers, athletic staff, medical staff, support staff, and other members of the organization, as all these individuals could contract the virus and ultimately affect the ability of the team and league to participate and succeed. To minimize the risk of spread in this way, an organization’s plan for return to play should include the following six pillars:
- Appropriate hygiene and physical distancing
- Use of masks
- Rigorous monitoring and screening of symptoms
- Widespread testing
- Comprehensive contact tracing
- Considerations for travel and facilities
Appropriate Hygiene and Physical Distancing
An essential method of preventing the spread of COVID-19, and any other respiratory viral illness, is to ensure athletes are washing their hands correctly and frequently (Güner et al., 2020). Athletes should be instructed on how to appropriately wash their hands, using either soap and water or an alcohol-based hand sanitizer containing at least 60% alcohol, as well as to avoid contact with their face and mouth after touching potentially contaminated surfaces (Golin et al., 2020). In addition, physical distancing can help reduce contact between any team members who have been infected with the virus but are asymptomatic, and those who have not been exposed to the virus (Güner et al., 2020). Effective measures for physical distancing involve keeping six feet (~2 meters) between athletes when possible, limiting nonessential visitors and spectators, and avoiding congregating in large groups (Playing Sports, CDC, 2020).
Use of Masks
Another tool to prevent the spread of COVID-19 is the use of masks. It is known that wearing a mask covering both the nose and mouth helps reduce the spread of COVID-19 between individuals (Playing Sports, CDC, 2020; Howard et al., 2021). A cloth mask is appropriate to avoid spread in the sports setting (Howard et al., 2021). In instances where it is not feasible for athletes to wear masks, such as with higher intensity sports and competition, the organization should work to make sure sports are taking place either outside or in a well-ventilated area (Playing Sports, CDC, 2020).
Rigorous Monitoring and Screening of Symptoms
To prevent COVID-19 from swiftly spreading among a team, it is important to rapidly identify individuals who may be infected with the virus. This can be done through daily self-reported screening for symptoms of COVID-19. One effective and efficient way to do this is through mobile applications (Zens et al., 2020). While this method may miss asymptomatic athletes, it can be used in conjunction with the other pillars described to prevent infection.
Widespread Testing
To detect asymptomatic or subclinical presentations of COVID-19, widespread testing is required. While the ability of different organizations to test depends on the level of sport and resources, at minimum all athletes should be tested prior to the start of the season. Simulations of air travel show that polymerase chain reaction (PCR) testing 72 hours prior to travel is an effective testing strategy for asymptomatic travelers, and as a result this timeframe has been widely adopted by different cities, states, and countries with regard to allowing visitors in (Kiang et al., 2021). We recommend a similar strategy for testing in nonvaccinated individuals prior to the beginning of a sporting match or event. If organizational resources allow, serial testing should also take place prior to competition.
Comprehensive Contact Tracing
If and when athletes test positive, it is important for organizations to have protocols in place for contact tracing, which is identifying individuals who may have been exposed to the virus and informing them of their need to isolate. Organizations should be meticulous in maintaining a list of everyone who is present at team events or in the facility, for contact tracing purposes. Depending on the level of sport or the event, there is also an opportunity to use technology, such as Bluetooth devices, mobile applications, or global positioning system (GPS) bracelets to identify athletes and staff who are high-risk contacts with a person who tests positive (Ryan et al., 2020). To minimize significant spread as well as complicated tracing procedures, implementing rigid seat assignments for team meals, travel movements, locker room and bench seating should be considered.
Consideration for Travel and Facilities
The increased emphasis on hygiene and physical distancing creates new challenges with regard to both the physical spaces that sports inhabit and how we travel to those spaces. It is important to clean and disinfect highly trafficked areas of the facility and be flexible in how we use our spaces, such as instituting one-way traffic areas to ensure proper physical distancing. Travel should only take place if the overall rates of infection for both the team and community are low and should follow directives from health officials. For team travel, accommodations should be made to ensure appropriate distancing between athletes, which may include increasing the number of vehicles or reducing the number of individuals traveling.
MODELS FOR RETURN TO PLAY
There have been a number of different models of return to play that are ultimately based on these six pillars, and most of these were first introduced in the professional sports arena. One model that was utilized was the bubble concept, most famously employed by the NBA. This involved suspending the season, then re-introducing the league into an isolated environment. Prior to rejoining the league, players were required to have two negative tests to enter the bubble (Bontemps, 2020), and once in the bubble, were required to abide by strict rules limiting socialization with other teams and requiring quarantine if any player left the bubble. This resulted in zero positive cases of COVID-19 for the duration of the NBA season in the bubble (Pegher, 2020).
Other less restrictive “controlled environment” models have been utilized in which players and staff live in their homes and continue to participate with screening, behavioral modifications, and serial testing. These models have had variations in testing frequency, with variable success in preventing COVID-19 in athletes (National Football League (NFL), 2020). One example was the Bundesliga league in Germany, where athletes, ball boys, referees, doping control officers, and TV personnel all had to complete daily symptom screening questionnaires. Each team also had a designated hygiene officer, who was a medical doctor, and players (and referees) were required to have two negative swabs within 5 days of beginning training camp, and two PCR tests every week. Of 1702 individuals tested, 8 players and 4 officials tested positive prior to training camp, 2 players tested positive during the third round of testing, and there were no further positive tests for the rest of the season. One caveat to this model is the need for the organization to be in tune with directives by state and local health officials, as the prevalence of COVID-19 in the community ultimately affects the risk of outbreaks on the team. In the absence of a completely isolated environment, a high prevalence of COVID-19 could mean members of the team may contract the disease outside sporting activities and cause outbreaks among the team.
The first professional sport in the United States to proceed in 2020 was the National Women’s Soccer League (NWSL), which hosted the Challenge Cup in June 2020, using a bubble format similar to that of the NBA. After success with the bubble format, the NWSL then moved to a “controlled environment” model later in the season. This highlighted the collaborations across leagues and medical officers operating as “incident commanders” during the pandemic.
YOUTH SPORTS
Youth sports offer a unique challenge for return to play for several reasons. For one, this level of sport is often tied to schools for participation. With school closures and the transition to virtual learning, in-person activities are dependent on local health directives and school boards, leading to a transition away from organized sports (Dunton et al., 2020). When in-person activities are allowed by local communities, an added challenge emerges. This level of sport has the highest risk of athletes contracting the disease outside of sporting activities and does not have sufficient funding or resources to perform widespread testing at the levels seen in professional sports. One model used by a youth soccer club in Washington state, Seattle United, involved dividing the team into pods of five individuals for practice and emphasized physical distancing, symptom monitoring, wearing masks when not exercising, and testing when athletes developed symptoms (Drezner et al., 2021). This resulted in only 2 players out of the 15,494 who practiced over the course of about one month testing positive. This study showed a model for keeping athletes safe and healthy with a focus on distancing, hygiene, masking, and symptom monitoring. However, this strategy is dependent on widespread access to testing in the community, to allow athletes to get tested if they do develop symptoms.
VACCINATIONS
A source of hope during the COVID-19 pandemic has been the rapid development of vaccinations, with the possibility that these will prevent disease and allow “normal” activities such as sport to resume. Several vaccines are currently approved for emergency use authorization by the Food and Drug Administration (FDA) in the United States, and rapid distribution of these vaccines has begun. According to the WHO, as of July 2021, a total of 2.9 billion doses of eleven different vaccines targeted against COVID-19 have been administered throughout the world, and as of May 2021, administration has been expanded to pediatric populations (WHO, 2021). The distribution of vaccines has been unequal geographically, resulting in some areas and populations having much greater protection than others. As the vaccine supply continues to rise across the globe and becomes more evenly distributed, it is fair to anticipate a “passport to participation” made up of full vaccination and/or negative PCR testing for return to sport, with a progressive decrease in restrictions as the percentage of vaccinated persons increases. However, it is important to note that vaccination does not replace the need for the six pillars of return to play described above. No vaccine is 100% effective at preventing disease, and with the rise of variants of COVID-19, there is a risk of illness after successful vaccination (Hacisuleyman et al., 2021). Despite this, vaccines remain our best method of protecting our athletes against COVID-19 infection, and from a public health perspective, widespread vaccination is our path to achieving herd immunity to COVID-19 and our road toward the end of the pandemic.
THE ROLE OF NUTRITION
Much like the aforementioned pillars of return to play and the implementation of vaccines, our goal is to prevent disease before it starts. In addition to emphasizing the need for physical distancing (when possible), widespread masking, and vaccination (when available), it is also important to emphasize the effects that nutrition can have on the immune system. On a macro level, the “Western” diet (high in processed, deep-fried, and high-fat foods) has been associated with the development of an inflammatory state, as well as hyperglycemia and other metabolic complications (Zabetakis et al., 2020). These effects could compound negative health outcomes in the setting of a pandemic, especially in one like COVID-19, where severe cases have been tied to a severe inflammatory response (Xie et al., 2020). Rather than the Western diet, athletes should be encouraged and empowered to consume foods with an adequate supply of energy from glucose, amino acids, and fatty acids to strengthen their immune system to resist disease, as well as obtain enough micronutrients to help mitigate against tissue damage during infection (Iddir et al., 2020; Walsh, 2019). There has been extensive evidence demonstrating the effects of micronutrients on infection, especially in viral infections such as COVID-19. Zinc has been shown to decrease upper respiratory illness (URI) duration, while both vitamin C and vitamin D have been shown to reduce the incidence of illness in athletes (Ali et al., 2020; Hemilä et al., 2013; Walsh, 2019). Specifically, with COVID-19, vitamin D levels have been correlated with incidence of COVID-19 in communities and whether hospitalized individuals require the intensive care unit or the general floor; however, the same correlation has not been seen with COVID-19 deaths (Ali et al., 2020). While there are still many unanswered questions, including if vitamin D supplementation is better used as prophylaxis or treatment, what the optimal levels of vitamin D are, and what populations can most benefit from supplementation, it is important as members of the sports medicine community that we recognize the effect nutrition has on our athletes in the setting of the COVID-19 pandemic. We need to emphasize the need to not only condition our athletes to avoid physical injury, but also focus on conditioning and optimizing the immune system through diet to help avoid illness.
PROTOCOLS FOR ATHLETES AFTER INFECTION
In addition to protocols to prevent infections and breakouts among team members, it is important to develop protocols for athletes who do contract the virus. Protocols were developed by the American College of Cardiology Sports and Exercise Leadership Council, as well as the United Kingdom, to identify post-COVID-19 myocarditis (Phelan et al., 2021; Wilson et al., 2020). These recommendations suggest that patients who test positive but are asymptomatic should have a two-week period of isolation and rest followed by a slow resumption to activity under the guidance of a healthcare team. For those athletes who have symptoms that do not require hospitalization, it is recommended they have a 10- to 14-day period of rest after resolution of symptoms, followed by an evaluation by a healthcare professional, including biomarker testing, electrocardiogram (EKG), and echocardiogram. Those who have more than 14 days of symptoms should also receive cardiac magnetic resonance (MR) imaging. If the results are normal, they should undergo exercise testing and 24-hour EKG Holter monitoring. Those who continue to have respiratory symptoms should have biomarker testing and a chest X-ray. Abnormal results should be confirmed by computerized tomography (CT) imaging of the chest or MR, and cardiopulmonary exercise testing if the CT is inconclusive. For those hospitalized, it is recommended to have biomarker testing and imaging performed during the hospitalization. If the in-hospital tests are unremarkable, patients should have a repeat evaluation completed two weeks after cessation of symptoms. If at any point the athlete has an abnormal cardiac test, they should follow myocarditis return-to-play guidelines (Maron et al., 2015).
SUMMARY
The COVID-19 pandemic demonstrated the importance of having an ICS at multiple levels of sport, from individual teams to national and multinational organizations, to efficiently and effectively make decisions around sport in the wake of unexpected occurrences, both natural and manmade. This structure is composed of a multidisciplinary team with clearly defined roles tailored to the specific incident and facilitates rapid communication of plans and policies. The pandemic highlighted the importance of ensuring medical professionals be part of these teams to help guide decisions surrounding medical and safety disasters such as this. As such, our recommendation is that all sports organizations involve a medical professional to aid in decision making as it pertains to the medical aspects of potential incidents.
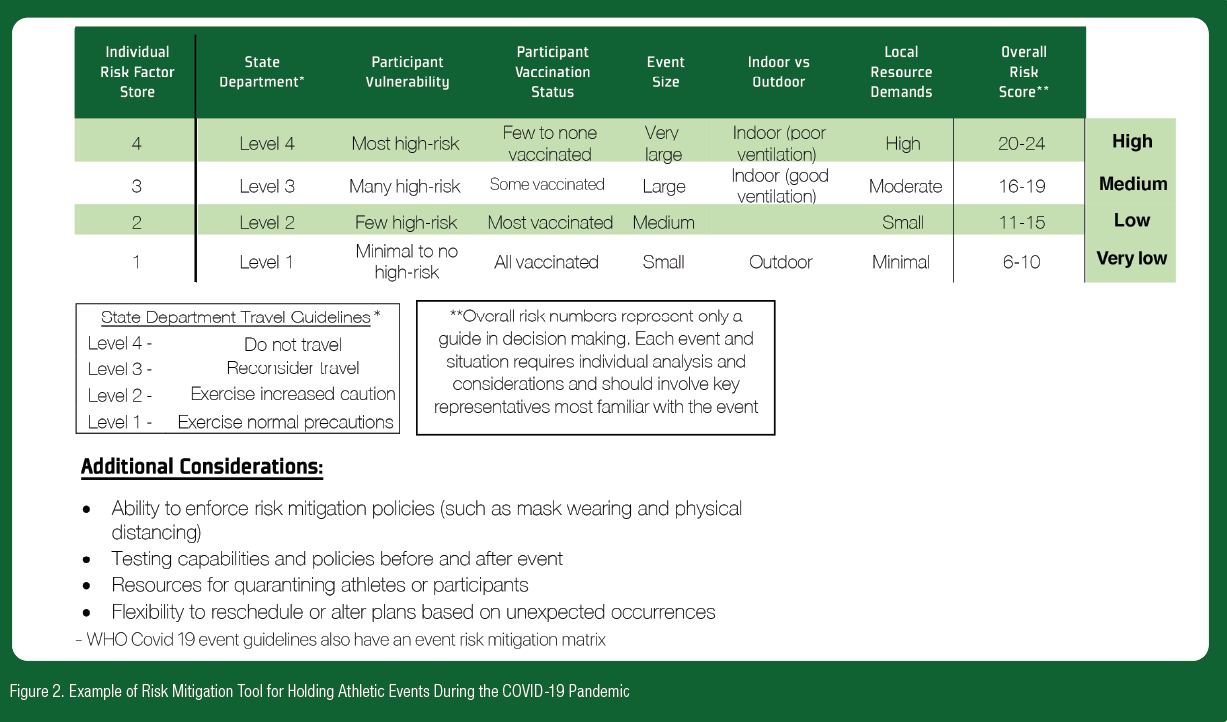
The COVID-19 pandemic also demonstrated the importance of having clear guidelines for preventing disease, as well as for return to play after disease. Some basic prevention guidelines are highlighted by our six pillars of return to play, as well as our recommendations that organizations encourage vaccination of athletes and other members of the organization (as well as fans and the general public) to prevent further outbreaks and spread, allowing for more normal sporting conditions, as well as encouraging proper nutrition to prevent and limit an inflammatory state. Return to play depends on the risk the event poses to both members of the organization and the public; risk assessment tools such as the one described in Figure 2 can be used to assess this risk. Models of return to play were largely adapted from the “bubble” and “controlled environment” concepts, first introduced by professional teams. A model for youth sports utilized a modified controlled environment concept and was successful in preventing disease in athletes and spread through the team.
For athletes who test positive for disease, guidelines for return to play are based on the risk for post-COVID-19 myocarditis, and our recommendations are adapted from the American College of Cardiology Sports and Exercise Leadership Council, as well as the United Kingdom. These can be found in our “summary of recommendations” (Figure 3).

Of note, these guidelines, both for reducing the spread of disease and reducing morbidity and mortality of athletes after infection, were partly formulated thanks to research during the pandemic that was collated into guidelines by healthcare professionals who were part of ICS. The collaboration between different sport organizations and researchers highlighted the importance of this structure to formulate guidelines for safe resumption of activities initially, and to return to a “normal” level of play recently. As vaccines continue to be further and more equitably distributed, this ICS will continue to be important to continually address both the changing landscape of the pandemic and further unexpected events in sport.
The views expressed are those of the authors and do not necessarily reflect the position or policy of PepsiCo, Inc.
REFERENCES
Ali, N. (2020). Role of vitamin D in preventing of COVID-19 infection, progression, and severity. J. Infect. Public Health 13:1373-1380.
Bontemps T. (2020). In documents, NBA details coronavirus testing protocols including 2-week resting period for positive tests. https://web.archive.org/web/20200924154012/https://www.epsn.com/nba/story/_id/29321006/in-documents-nba-details-coronavirus-testing-process-orlando-campus-life. Published June 16, 2020. Accessed December 10, 2020.
Centers for Disease Control and Prevention (2020). Estimated influenza illnesses, medical visits, hospitalizations, and deaths in the United States 2018-2019 influenza season. https://www.cdc.gov/flu/about/burden/2018-2019.html. Published 2020. Updated January 8, 2020. Accessed December 10, 2020.
Centers for Disease Control and Prevention (2020). Playing Sports. https://www.cdc.gov/coronavirus/2019-ncov/daily-life-coping/playing-sports.html. Published 2020. Updated December 31, 2020. Accessed May 01, 2021.
Centers for Disease Control and Prevention (2020). Ways COVID-19 Spreads. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html. Published 2020. Updated October 28, 2020. Accessed May 01, 2021.
Drezner, J.A., S.M. Drezner, K.N. Magner, and J.Y. Ayala (2021). COVID-19 surveillance in youth soccer during small group training: A safe return to sports activity. Sports Health 13:15-17.
Dunton, G.F., B. Do, and S.D. Wang (2020). Early effects of the COVID-19 pandemic on physical activity and sedentary behavior in children living in the U.S. BMC Public Health 20:1351.
Federal Emergency Management Agency (FEMA). Glossary. https://training.fema.gov/programs/emischool/el361toolkit/glossary.htm. Accessed June 12, 2021.
Golin, A.P., D. Choi, and A. Ghahary (2020). Hand sanitizers: A review of ingredients, mechanisms of action, modes of delivery, and efficacy against coronaviruses. Am. J. Infect. Control 48:1062-1067.
Güner, R., I. Hasanoğlu, and F. Aktaş (2020). COVID-19: Prevention and control measures in community. Turk. J. Med. Sci. 50:571-577.
Guan, W.J., Z.Y. Ni, Y. Hu, W.H. Liang, C.Q. Ou, J.X. He, L. Liu, H. Shan, C.L. Lei, D.S.C. Hui, B. Du, L.J. Li, G. Zeng, K.Y. Yuen, R.C. Chen, C.L. Tang, T. Wang, P.Y. Chen, J. Xiang, S.Y. Li, J.L. Wang, Z.J. Liang, Y.X. Peng, L. Wei, Y. Liu, Y.H. Hu, P. Peng, J.M. Wang, J.Y. Liu, Z. Chen, G. Li, Z.J. Zheng, S.Q. Qiu, J. Luo, C.J. Ye, S.Y. Zhu, and N.S. Zhong; China Medical Treatment Expert Group for Covid-19 (2020). Clinical characteristics of coronavirus disease 2019 in China. N. Engl. J. Med. 382:1708-1720.
Hacisuleyman, E., C. Hale, Y. Saito, N.E. Blachere, M. Bergh, E.G. Conlon, D.J. Schaefer-Babajew, J. DaSilva, F. Muecksch, C. Gaebler, R. Lifton, M.C. Nussenzweig, T. Hatziioannou, P.D. Bieniasz, and R.B. Darnell (2021) Vaccine breakthrough infections with SARS-CoV-2 variants. N. Engl. J. Med. 384:2212-2218.
Hemilä, H., and E. Chalker (2013). Vitamin C for preventing and treating the common cold. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.cd000980.pub4.
Howard, J., A. Huang, Z. Li, Z. Tufekci, V. Zdimal, H.M. van der Westhuizen, A. von Delft, A. Price, L. Fridman, L.H. Tang, V. Tang, G.L. Watson, C.E. Bax, R. Shaikh, F. Questier, D. Hernandez, L.F. Chu, C.M. Ramirez, and A.W. Rimoin (2021). An evidence review of face masks against COVID-19. Proc. Natl. Acad. Sci. USA 118:e2014564118.
Iddir, M., A. Brito, G. Dingeo, S.S. Fernandez Del Campo, H. Samouda, M.R. La Frano, and T Bohn (2020). Strengthening the immune system and reducing inflammation and oxidative stress through diet and nutrition: Considerations during the COVID-19 crisis. Nutrients 12:1562.
Kiang, M.V., E.T. Chin, B.Q. Huynh, L.A.C. Chapman, I. Rodríguez-Barraquer, B. Greenhouse, G.W. Rutherford, K. Bibbins-Domingo, D. Havlir, S. Basu, and N.C. Lo (2021). Routine asymptomatic testing strategies for airline travel during the COVID-19 pandemic: a simulation analysis. Lancet Infect. Dis. Mar 22:S1473-3099(21)00134-1. Online ahead of print.
Li, Q., X. Guan, P. Wu, X. Wang, L. Zhou, Y. Tong, R. Ren, K.S.M. Leung, E.H.Y. Lau, J.Y. Wong, X. Xing, N. Xiang, Y. Wu, C. Li, Q. Chen, D. Li, T. Liu, J. Zhao, M. Liu, W. Tu, C. Chen, L. Jin, R. Yang, Q. Wang, S. Zhou, R. Wang, H. Liu, Y. Luo, Y Liu, G. Shao, H. Li, Z. Tao, Y. Yang, Z. Deng, B. Liu, Z. Ma, Y. Zhang, G. Shi, T.T.Y. Lam, J.T. Wu, G.F. Gao, B.J. Cowling, B. Yang, G.M. Leung, and Z. Feng (2020). Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia. N. Engl. J. Med. 382:1199-1207.
Maron, B.J., J.E. Udelson, R.O. Bonow, R.A. Nishimura, M.J. Ackerman, N.A.M. Estes 3rd, L.T. Cooper Jr, M.S. Link, and M.S. Maron (2015). Eligibility and disqualification recommendations for competitive athletes with cardiovascular abnormalities: Task Force 3: Hypertrophic Cardiomyopathy, Arrhythmogenic Right Ventricular Cardiomyopathy and other Cardiomyopathies, and Myocarditis: A scientific statement from the American Heart Association and American College of Cardiology. J. Am. Coll. Cardiol. 66:2362-2371
National Incident Management System (NIMS) (2017) In: United States. Federal Emergency Management Agency.
National Football League (NFL) COVID-19 Protocols (2020). NFL Football Operations. https://operations.nfl.com/football-ops/nfl-covid-19-protocols/. Published 2020. Accessed December 10, 2020.
Osburn, S. (2020, March 17). NCAA cancels remaining winter and spring championships. NCAA.org - The Official Site of the NCAA. https://www.ncaa.org/about/resources/media-center/news/ncaa-cancels-remaining-winter-and-spring-championships.
Pegher, K. (2020). Coronavirus Today: The NBA’s bubble worked. Los Angeles Times, October 12, 2020.
Phelan, D., J.H. Kim, and E.H. Chung (2021). A game plan for the resumption of sport and exercise after coronavirus disease 2019 (COVID-19) infection. J. Am. Med. Assoc. Cardiol. 6:479-480.
Ryan, B.J., D. Coppola, J. Williams, and R. Swienton (2020). COVID-19 contact tracing solutions for mass gatherings. Disaster Med. Public Health Prep. 14:1-7.
Walsh, N.P. (2019). Nutrition and athlete immune health: New perspectives on an old paradigm. Sports Med. 49(Suppl 2):153-168.
Wilson, M.G., J.H. Hull, J. Rogers, N. Pollock, M. Dodd, J. Haines, S. Harris, M. Loosemore, A. Malhotra, G. Pieles, A. Shah, L. Taylor, A, Vyas, F.S. Haddad, and S. Sharma (2020). Cardiorespiratory considerations for return-to-play in elite athletes after COVID-19 infection: a practical guide for sport and exercise medicine physicians. Br. J. Sports Med. 54:1157-1161.
World Health Organization. (2020), Coronavirus disease (COVID-19). https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub/q-a-detail/coronavirus-disease-covid-19. Published 2020. Updated October 12, 2020. Accessed December 10, 2020.
World Health Organization. (2021). Coronavirus disease (COVID-19): Vaccines. https://www.who.int/news-room/q-a-detail/coronavirus-disease-(covid-19)-vaccines Published October 28, 2020. Updated April 8, 2021. Accessed May 1, 2021.
Xie, P., W. Ma, H. Tang H, and D. Liu (2020). Severe COVID-19: A review of recent progress with a look toward the future. Front. Public Health 8:189.
Zabetakis, I., R. Lordan, C. Norton, and A. Tsoupras (2020). COVID-19: The inflammation link and the role of nutrition in potential mitigation. Nutrients 12:1466.
Zens, M., A. Brammertz, J. Herpich, N. Südkamp, and M. Hinterseer (2020). App-based tracking of self-reported COVID-19 symptoms: Analysis of questionnaire data. J. Med. Internet. Res. 22:e21956.








