Hydration Assessment of Athletes
Published
October 2006
Author
Samuel N. Cheuvront, Ph.D., Michael N. Sawka, Ph.D. FACSM
Topics

Key Terms
- Although there is no scientific consensus for 1) how best to assess the hydration status of athletes, 2) what criteria to use as acceptable outcome measurements, or 3) the best time to apply practical assessment methods, there are methods that can be used to provide athletes with useful feedback about their hydration status
- Hydration assessment techniques include 1) total body water measured by isotope dilution or estimated by bioelectrical impedance analysis, 2) plasma markers, such as osmolality,sodium, hematocrit and hemoglobin changes, or the concentrations of hormones that help regulate body fluids, 3) urine markers, such as osmolality, specific gravity, or color, 4) changes in body mass, and 5) other variables, such as salivary flow or gross, physical signs and symptoms of clinical dehydration.
- In most athletic settings, the use of body mass measurements in combination with some measure of urine concentration at the first urination of the morning allows ample sensitivity for detecting daily deviations from normal hydration (euhydration). The methods are simple, inexpensive, accurately distinguish euhydration from dehydration,and can therefore be used as a sole source for assessment.
- When more precision of acute hydration changes is desired, plasma osmolality, isotope dilution, and body mass changes, used in appropriate context, provide for the accurate gradations in measurement often required in research.
- Plasma markers (other than osmolality), bioelectrical impedance analysis, saliva measures, and gross physical signs and symptoms of dehydration are often confounded or too inaccurate to reliably assess hydration of athletes.
INTRODUCTION
Body water balance represents the net difference between fluid intake and loss. Normal body water turnover in a sedentary adult is from 1 to 3 L/day, the range accountable primarily to differences in insensible water loss, or the evaporation of moisture from the skin (Sawka et al., 2005). Large variations in fluid intake are controlled by the kidneys, which can produce more or less urine, depending on changes in body fluid volumes. Water loss in air exhaled from the lungs is often ignored with respect to water balance because it is usually offset by water production occurring during aerobic metabolism (Sawka et al., 2005). Over the course of a day, humans usually regulate daily bodywater balance remarkably well as a result of thirst and hunger drives coupledwith free access to food and beverage. This is accomplished by physiological responses to changes in body water volume and to changes in concentrations of dissolved substances in body fluids, as well as by non-regulatory social-behavioral factors, such as drinking fluids at meetings and parties (Sawka et al., 2005).
Although minor perturbations in daily body water balance are easily restored to normalcy, the imposition of exercise and environmental stress onto daily activity can seriously threaten fluid balance homeostasis, performance, and health (Panel on DRI., 2005). Abating these consequences is the underlying and unifying basis for developing guidelines for fluid intake before, during, and after exercise (Casa et al., 2000; Convertino et al., 1996), but hydration assessment remains a key component for ensuring full rehydration in athletes performing frequent and intense exercise in hot weather.
The selection of an appropriate hydration assessment method is a controversial aspect of fluid balance science (Oppliger & Bartok, 2002). All hydration assessment techniques vary greatly in their applicability due to methodological limitations such as the necessary circumstances for measurement (reliability),ease and cost of application (simplicity), sensitivity for detecting small, but meaningful changes in hydration status (accuracy), and the type of dehydration anticipated (Oppliger & Bartok, 2002; Sawka et al., 2005).
Most circumstances involving strenuous physical exercise require the formation and vaporization of sweat as a principal means of heat removal. When sweat losses produce a body water deficit, the reduced volume of body fluids contains a greater than normal concentration of dissolved substances such as sodium and potassium; this is known as hypertonic hypovolemia, the norm for dehydrated athletes (Sawka & Coyle, 1999). Clinical hydration assessment techniques for detecting changes in hydration status rely heavily on this alteration in body fluid chemistry.
RESEARCH REVIEW
Objectives and Definitions
The purposes of this paper are to: 1) evaluate several common methods for assessing hydration status, 2) provide acceptable outcome criteria for the most accurate and reliable methods, and 3) offer application guidance for athletes and coaches. Because considerable latitude is given when using terms common to hydration research, we define two here for clarity. "Euhydration" is a dynamicprocess rather than a static set-point (Greenleaf, 1992). It is most accurately defined as a normal total body water that fluctuates narrowly. Although dehydration and hypohydration have unique definitions, they are often used interchangeably as their differences are subtle. For this review, the more common term "dehydration" will be used in reference to a body water deficit.
Assessment Techniques
Complex Markers
Population estimates of fluid needs are based on qualitative and quantitative data (Sawka et al., 2005). Fluid intake surveys provide qualitative data, whereas water balance studies and biochemical assessments offer quantitative support for the adequacy of reported intakes. The combination of total body water and plasma osmolality provides the "gold standard" for hydration assessment.
Total Body Water. The process of measuring water balance by collecting input and output data has been modernized by estimating total body water (TBW), which entails measuring the dilution of trace amounts of an isotope (usually deuterium oxide, 2H2O). The details, assumptions, and limitations behind isotope dilution have been discussed elsewhere, but the accuracy of this method closely approximates values measured by desiccation, i.e., the slow heating of cadaver tissue until all water is removed (Ritz, 1998). In brief, a known volume and concentration of isotope is taken into the body, and a new concentration of the isotope is later determined in a sample of body fluid (blood, saliva, etc.) after the tracer has become distributed equally throughout the body fluids. The unknown volume (TBW) is then calculated, knowing that a low concentration of the isotope in the sample means that the body fluid volume must be relatively large and vice versa. Like other quantitative techniques, isotope dilution does not allow determination of an adequate baseline due to the wide variability in body composition and associated variability in normal total body water (Panel DRI 2005). However, the total error of measuring TBW with tracer dilution is as low as 1% (Ritz, 1998), thus allowing measurement of small changes in body fluids.
Plasma Osmolality. Plasma osmolality is controlled around a euhydration set-point of ~285 mOsm/kg (Panel DRI 2005). Exercise sweat losses, if not replaced, reduce body water volume. Plasma volume and extracellular water decrease because they provide the fluid for sweat, and plasma osmolality increases because sweat is hypotonic relative to plasma. In other words, sweat removes relatively more water from body fluids than solutes like sodium and chloride, and these osmotically active solutes build up in the blood plasma. The increase in plasma osmotic pressure is proportional to the decrease in total body water (Panel DRI 2005). Popowski et al. (2001) demonstrated under well-controlled conditions that plasma osmolality increases by ~5 mOsm/kg for every ~ 2% loss of body mass by sweating. Importantly, they also showed that plasma osmolality returns toward normal values during rehydration. Although field studies sometimes do not demonstrate this relationship, the discrepancy can be explained by environmental confounders such as altitude (Francesconi et al., 1987) or by small changes in hydration status (< 2% body mass) (Armstrong et al., 1994; Bergeron et al.,1995; Grandjean et al., 2003) that may fall within the normal fluctuating range for euhydration (Greenleaf, 1992).
These "gold standards" of hydration assessment are good for sports science, medicine, or for establishing reference criteria, but because they require considerable methodological control, expense, and analytical expertise, they are not of practical use for monitoring day-to-day hydration status during training or competition. Table 1 should be consulted when choosing a complex hydration marker.
Simple Markers
Urine Concentration. Urinalysis is a frequently used clinical measure to distinguish between normal and pathological conditions. Urinary markers for dehydration include a reduced urine volume, a high urine specific gravity (USG), a high urine osmolality (UOsm), and a dark urine color (UCol). Urine is a solution of water and various other substances, and the concentration of those substances increases with a reduction in urine volume, which is associated with dehydration. Urine output is roughly 1 to 2 liters per day but can be increased 10-fold when consuming large volumes of fluid (Sawka et al.,2005). This large capacity to vary urine output represents the primary avenue to regulate net body water balance across a broad range of fluid intake volumes and fluid losses from other avenues. Although it is impractical to measure urine volume on a daily basis, the quantitative (USG, UOsm) or qualitative (UCol) assessment of its concentration is far simpler. As a screening tool to differentiate euhydration from dehydration, urine concentration as indicated by USG, UOsm, or UCol is a reliable assessment technique (Armstrong et al., 1994; Bartok et al.,2004; Shirreffs & Maughan, 1998) with reasonably definable thresholds.
In contrast, urine measures often correlate poorly with "gold standards" like plasma osmolality and fail to reliably track documented changes in body mass corresponding to acute dehydration and rehydration (Kovacs et al., 1999; Popowski et al., 2001). It appears that changes in plasma osmolality that stimulate endocrine regulation of the reabsorption of renal water and electrolytes are delayed at the kidney when acute changes in body water occur (Popowski et al., 2001). It is also likely that drink composition influences this response. Shirreffs and Maughan (1996) demonstrated that drinking large volumes of dilute (hypotonic) fluids results in copious urine production long before euhydration is achieved. Urine concentration measurements can also be confounded by diet, which may explain large cross-cultural differences in urine osmolality (Manz & Wentz, 2003). However, use of a sample from the first void (urination) of the morning following an overnight fast minimizes confounding influences and maximizes measurement reliability (Armstrong et al., 1994; Fischbach,1992; Shirreffs & Maughan, 1998). Analysis of urinary specific gravity,osmolality, and color can therefore be used to assess and distinguish euhydration from dehydration so long as the first void in the morning is used.
Body Mass. Body mass is often used to assess the rapid changes of athlete hydration in both laboratory and field environments. Acute changes in hydration are calculated as the difference between pre- and post-exercise body mass. The level of dehydration is best expressed as a percentage of starting body mass rather than as a percentage of TBW because the latter varies widely (Sawkaet al., 2005). Use of this technique implies that 1 g of lost mass is equivalent to 1 ml of lost water. So long as total body water loss is of interest, failure to account for carbon exchange in metabolism represents the only small error in this assumption (Cheuvront et al., 2002). Indeed, acute changes in body mass (water) are frequently the standard against which the resolution of other hydration assessment markers is compared in the laboratory. In fact, if proper controls are made, body mass changes can provide a more sensitive estimate of acute changes in total body water than repeated measurements by dilution methods (Gudivaka et al., 1999).
There is also evidence that body mass may be a sufficiently stable physiological marker for monitoring daily fluid balance, even over longer periods (1-2-wks) that include hard exercise and acute fluid changes (Cheuvront et al., 2004; Leiperet al., 2001). Young, healthy men undergoing daily exercise and heat stress maintain a stable body mass when measured first thing in the morning as long as they make a conscious effort to replace sweat lost during exercise (Cheuvrontet al., 2004). Similarly, voluntary intakes of food and fluid compensate for sweat losses incurred with regular exercise, resulting in a stable daily body mass (Leiper et al., 2001). Over longer periods, changes in body composition (fat and lean mass) that occur with chronic energy imbalance are also reflected grossly as changes in body mass, thus limiting this technique for assessment of hydration. Clearly, if long-term hydration status is of interest and stability of body mass measured after awakening in the morning is used to monitor changes in hydration, body mass measurements should be used in combination with another hydration assessment technique (urine concentration) to dissociate gross tissue losses from water losses.
Simple markers of hydration status afford athletes or coaches the ability to monitor daily fluid balance. Relatively inexpensive and easy-to-use commercial instruments are available for assessing urine specific gravity and conductivity (an osmolality equivalent) (Bartok et al., 2004, Shirreffs & Maughan,1998). A urine color chart is also available (Armstrong et al., 1994). So long as nude body mass is measured, almost any scale is suitable for self-monitoring of body mass, although a kilogram balance or medical-grade scale manufactured in accordance with international weighing standards is preferred. Table 1 summarizes the strengths and weaknesses of using simple hydration markers.
|
Table 1. Hydration assessment techniques summary. |
||
|
Technique |
Advantages |
Disadvantages |
|
Complex Markers |
||
|
Total Body Water (dilution) |
Accurate, reliable (gold standard) |
Analytically complex, expensive, requires baseline |
|
Plasma Osmolality |
Accurate, reliable (gold standard) |
Analytically complex, expensive, invasive |
|
Simple Markers |
||
|
Urine Concentration |
Easy, rapid, screening tool |
Easily confounded, timing critical, frequency and color subjective |
|
Body Mass |
Easy, rapid, screening tool |
Confounded over time by changes in body composition |
|
Other Markers |
||
|
Blood: |
||
|
Plasma volume Plasma Sodium Fluid Balance Hormones |
No advantages over osmolality (except hyponatremia detection for plasma sodium) |
Analytically complex, expensive, invasive, multiple confounders |
|
Bioimpedance |
Easy, rapid |
Requires baseline, multiple confounders |
|
Saliva |
Easy, rapid |
Highly variable, immature marker, multiple confounders |
|
Physical Signs |
Easy, rapid |
Too generalized, subjective |
|
Thirst |
Positive symptomology |
Develops too late and is quenched too soon |
Other Markers
Other hydration markers have also been investigated. The limitations of these methods are outlined in Table 1. The following is a brief discussion of their potential.
Other Blood Markers. Blood-borne markers of hydration other than osmolality include plasma volume, plasma sodium, and concentrations of fluid regulatory hormones in plasma. Under controlled conditions (exercise, temperature, posture), most plasma markers reliably measure changes in hydration. Plasma volume decreases proportionally with the level of dehydration, but this magnitude of change is markedly less in heat-acclimatized athletes (Sawka & Coyle, 1999). Plasma volume changes can be estimated from hemoglobin and hematocrit, but accurate measurement of these variables requires considerable controls for posture, arm position, skin temperature, and other factors (Sawka & Coyle, 1999). Plasma sodium provides an alternative to measuring osmolality because osmolality changes are primarily a reflection of sodium changes (Costill, 1977), but the relationship between hydration and plasma sodium is more variable than that between hydration and osmolality (Bartok et al., 2004; Senay, 1979). Fluid regulatory hormones, such as arginine-vasopressin and aldosterone, generally respond predictably to changes in body fluid volume and osmolality, but the hormones are easily altered by exercise and heat acclimation (Francesconi et al., 1983; Montain et al., 1997) and require more expensive and complicated analysis techniques. Although all plasma markers for hydration assessment involve blood sampling with varying degrees of subsequent analytical difficulty, plasma osmolality is the simplest, most accurate and reliable plasma marker for tracking hydration changes.
Bio-Impedance. Bioelectrical impedance analysis (BIA) is a noninvasive technique that can be used to estimate TBW. It uses low amperage current (single or multiple frequency) passed between skin electrodes with the assumption that current resistance (impedance) varies inversely with tissue water and electrolyte content. BIA is well correlated with TBW measures made using isotope dilution (O'Brien et al., 2002) under controlled laboratory conditions in euhydrated subjects. Although BIA is sensitive for detecting hypertonic hypovolemia, it significantly underestimates the level of absolute fluid losses and is independently altered by changes in body fluid volume and tonicity (O'Brien et al., 2002). Shifts of body fluids between intracellular and extracellular compartments during exercise, sweating, rehydration, and other variables common to athletic situations also confound its accuracy and make BIA unacceptable to monitor changes in hydration status (Panel DRI 2005).
Saliva and Symptoms. Salivais not as widely studied as other body fluids for potential monitoring of hydration, but salivary osmolality appears to track changes in hydration brought on by sweating. However, individual responses of saliva osmolality to changes in hydration are somewhat more variable than those for urine and much more variable than those for plasma (Walsh et al., 2004). Large variability in salivary flow has also been observed (Walsh, 2004), and salivary flow, like many other measures, also offers no clear trend at low levels of dehydration (Ship & Fisher, 1999). Salivary specific gravity increases with dehydration, but the variability is too great for quantitative analyses (Panel DRI 2005). Importantly, the influence of common food and beverage intake and oral hygiene practices on saliva indices has not been investigated.
Clinical signs and symptoms of dehydration, such as dizziness, headache, tachycardia,and others are far too generalized to be of predictive use, while more severe symptoms, such as delirium or deafness, occur at dehydration levels outside the functional range for training athletes. Although genuine thirst develops only after dehydration is present and is alleviated before euhydration is achieved (Panel DRI 2005), thirst is a useful symptom that draws attention to the need for more structured drinking before, during, or after exercise. Table 1 reviews the circumstantial limitations of choosing other markers to assess athlete hydration.
SUMMARY AND APPLICATIONS
Although plasma osmolality and total body water measurements are currently the best hydration assessment measures for large-scale assessment surveys of fluid needs (Sawka etal., 2005), there is presently no consensus for using any one approach over another in an athletic setting. In most circumstances, the use of body mass measured upon awakening in the morning combined with some measure of urine concentration (USG, UOsm, UCol) in a sample collected during the first void of the morning offers a simple assessment method and allows ample sensitivity for detecting meaningful deviations in fluid balance (> 2% body mass) for training and competing athletes. When more precision of acute hydration changes is desired, such as in the laboratory, plasma osmolality, isotope dilution,and acute changes in body mass allow gradations in measurement so long as proper techniques are used. Table 2 provides definable thresholds for the complex and simple markers of hydration recommended in this review for guidance in distinguishing euhydration from dehydration (Armstrong et al., 1994; Bartoket al., 2004; Casa et al., 2000; Cheuvront et al., 2004; Popowski et al., 2001;Ritz, 1998; Panel DRI 2005; Senay, 1979; Shirreffs and Maughan, 1998). Fluid balance should be considered adequate when any two assessment outcomes are consistent with euhydration thresholds.
|
Table 2. Recommended hydration assessment index thresholds |
||
|
Assessment Technique |
Athlete Practicality |
Acceptable Euhydration Cut-Off |
|
Change in Total Body Water ( L) |
Low |
|
|
Plasma Osmolality (mOsm) |
Medium |
|
|
Urine Specific Gravity (g/ml) |
High |
|
|
Urine Osmolality (mOsm) |
High |
|
|
Urine Color (#) |
High |
|
|
Change in Body Mass (kg) |
High |
|
|
Fluid balance should be considered adequate when the combination of any two assessment outcomes is consistent with euhydration. |
||
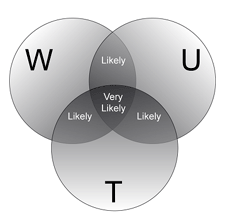
Based upon this review of the literature, an even simpler approach for self-monitoring of day-to-day hydration changes is proposed for athletes. This approach is represented using a Venn Diagram decision tool (Figure 1). It combines three of the simplest markers of hydration, including weight, urine, and thirst (WUT). No marker by itself provides enough evidence of dehydration, but the combination of any two simple self-assessment markers means dehydration is likely. The presence of all three makes dehydration very likely. The detailsfor using this diagram are provided in the accompanying Sports ScienceExchange Supplement.
Acknowledgement. The opinions or assertions contained herein are the private views of the authors and should not to be construed as official or reflecting the views of the Army or the Department of Defense. Approved for public release: distribution is unlimited.
REFERENCES
Armstrong, L.E., C.M. Maresh, J.W. Castellani, M.F. Bergeron, R.W. Kenefick, K.E. LaGasse, and D. Riebe, D. (1994). Urinary indices of hydration status. Int. J.Sport Nutr. 4:265-279.
Bartok, C., D.A. Schoeller, J.C. Sullivan, R.R. Clark, and G.L. Landry (2004). Hydration testing in collegiate wrestlers undergoing hypertonic dehydration. Med. Sci. Sports Exerc. 36:510-517.
Bergeron, M., C.M. Maresh, L.E. Armstrong, J. Signorile, J.W. Castellani, R.W. Kenefick, K.E. LaGasse, and D. Riebe (1995). Fluid-electrolyte balance associated with tennis match play in a hot environment. Int. J. Sport Nutr. 5: 180-193.
Casa, D.J., L.E. Armstrong, S.K. Hillman, S.J. Montain, R.V. Reiff, B.S.E. Rich, W.O. Roberts, and J.A. Stone (2000). National Athletic Trainers' Association position statement: fluid replacement for athletes. J. Athl. Train. 35:212-224.
Cheuvront, S.N., E.M. Haymes, and M.N. Sawka (2002). Comparison of sweat loss estimates for women during prolonged high-intensity running. Med. Sci. Sports Exerc. 34: 1344-1350.
Cheuvront S.N., R. Carter III, S.J. Montain, and M.N. Sawka (2004). Daily body mass variability and stability in active men undergoing exercise-heat stress. Int. J. Sport Nutr. Exerc. Metab. 14: 532-540.
Convertino, V.A., L.E. Armstrong, E.F. Coyle, G.W. Mack, M.N. Sawka, L.C. Senay and W.M. Sherman (1996). American College of Sports Medicine Position Stand: Exercise and fluid replacement. Med. Sci. Sports Exerc. 28: i - vii.
Costill, D.L. (1977). Sweating: its composition and effects on body fluids. Ann. N.Y. Acad. Sci. 301:160-174.
Fischbach, F. (1992). A Manual of Laboratory & Diagnostic Tests. 4thEd., Philadelphia: J.B. Lippincott Co., pp.138-224.
Francesconi, R.P., R.W. Hubbard, P.C. Szlyk, D. Schnakenberg, D. Carlson, N. Leva, I. Sils, L. Hubbard, V. Pease, A.J. Young, and D. Moore (1987). Urinary and hematological indexes of hydration. J. Appl. Physiol., 62: 1271-1276.
Francesconi, R.P., M.N. Sawka and K.B. Pandolf (1983). Hypohydration and heat acclimation:plasma renin and aldostrone during exercise. J. Appl. Physiol., 55:1760-1794, 1983.
Grandjean, A.C., K.J. Reimers, M.C. Haven, G.L. Curtis (2003). The effect on hydration of two diets, one with and one without plain water. J. Am. Coll. Nutr. 22:165-173.
Greenleaf, J.E. (1992). Problem: thirst, drinking behavior, and involuntary dehydration. Med. Sci. Sports Exerc. 24: 645-656.
Gudivaka, R., D.A. Schoeller, R.F.Kushner, and M.J.G. Bolt (1999). Single- and multi-frequency models for bioelectrical impedance analysis of body water compartments. J. Appl.Physiol. 87:1087-1096.
Kovacs, E.M., J.M. Senden, and F. Brouns (1999). Urine color, osmolality and specific electrical conductance are not accurate measures of hydration status during postexercise rehydration. J. Sports Med. Phys. Fit. 39: 47-53.
Leiper J., Y. Pitsiladis, and R.J. Maughan (2001). Comparison of water turnover rates in men undertaking prolonged cycling exercise and sedentary men. Int. J. Sports Med. 22:181-185.
Manz, F.and A. Wentz (2003). 24-h hydration status: parameters, epidemiology, and recommendations. Eur. J. Clin. Nutr. 57(suppl 2):S10-S18.
Montain, S.J., J.E. Laird, W.A. Latzka and M.N. Sawka (1997). Aldosterone and vasopressin responses in the heat: hydration level and exercise intensity effects. Med.Sci. Sports Exerc., 29:661-668.
O'Brien, C., A.J. Young, and M.N. Sawka (2002). Bioelectrical impedance to estimate changes in hydration status. Int. J. Sports Med. 23:361-366.
Oppliger, R.A. and C. Bartok (2002). Hydration testing for athletes. Sports Med. 32:959-971.
Panel on Dietary Reference Intakes for Electrolytes and Water. Chapter 4, Water, In: Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. Washington, D.C.: Institute of Medicine, National Academy Press, pp. 73-185, 2005.
Popowski, L.A., R.A. Oppliger, G.P. Lambert, R.F. Johnson, A.K. Johnson, and C.V. Gisolfi (2001). Blood and urinary measures of hydration during progressive acute dehydration. Med.Sci. Sports Exerc. 33:747-753.
Ritz, P. (1998). Methods of assessing body water and body composition. In: Hydration Throughout Life. Arnaud, M.J. (ed). Vittel: Perrier Vittel Water Institute, pp.63-74.
Sawka, M.N., S.N. Cheuvront, and R. Carter III (2005). Human water needs. Nutrition Reviews, 63(6): S30-39, 2005
Sawka, M.N.and E.F. Coyle (1999). Influence of body water and blood volume on thermoregulation and exercise performance in the heat. Exerc. Sports Sci.Rev. 27:167-218.
Senay, L.C., Jr. (1979). Effects of exercise in the heat on body fluid distribution. Med. Sci. Sports Exerc. 11:42-48.
Ship, J.A. and D.J. Fischer (1999). Metabolic indicators of hydration status in the prediction of parotid salivary-gland function. Arch. Oral Biol. 44:343-350.
Shirreffs, S.M. and R.J. Maughan (1998). Urine osmolality and conductivity as indices of hydration status in athletes in the heat. Med. Sci. Sports Exerc. 30:1598-1602.
Shirreffs, S.M and R.J. Maughan (1996). Post-exercise rehydration in man: effects of volume consumed and drink sodium content. Med. Sci. Sports Exerc. 28:1260-1271.
Walsh, N.P., S.J. Laing, S.J. Oliver, J.C. Montague, R. Walters and J.L.J. Bilzon (2004). Saliva parameters as potential indices of hydration status during acute dehydration. Med. Sci. Sports Exerc. 36:1535-1542.
Sports Science Exchange 97
VOLUME 18 (2005) NUMBER 2
SUPPLEMENT
Hydration Assessment ofAthletes
"WUT" IS the Answer?
"WUT" is amemory device designed to simplify athlete self-monitoring of day-to-dayhydration status. The concept for "WUT" is based on sound scientificprinciples of hydration assessment, but purposely requires nothing more than a body-weightscale. If adherence to fluid intake recommendations does not remedy suspecteddehydration using "WUT," or more objective measurement outcomes, such as plasmaosmolality or urine osmolality, should be used to confirm dehydration.
W stands for "weight." Athletes should maintain a day-to-day stablebody weight when measured first thing in the morning so long as they have freeaccess to food and beverage and replace sweat lost during exercise inaccordance with recommended fluid intake recommendations. Day-to-day bodyweight losses in excess of 1% may be an indication of dehydration. This is a day-to-dayloss of 1 lb (0.45 kg) for an athlete who weighs 100 lb (45.5 kg), 2 lbs (0.91kg) for an athlete weighing 200 lb (91 kg), or 3 lbs (1.4 kg) for an athleteweighing 300 lb (136.4 kg). Combine body weight information with thirst orchanges in urine (see Venn Diagram) to be more certain.
U stands for "urine". It is normalto produce more urine when body water is high and less urine when body water islow. Therefore, urine volume is generally more related to body water orhydration level than to drinking pattern. So if sweat losses are high, lessurine may be produced despite normal or even increased fluid intakes. Lowurine production can cause it to be more concentrated and a darker color. Areduced daily urine frequency and darkening of urine color in a sample takenduring the first urination of the morning may be an indication of dehydration. Combine urine information with information on thirst or body weight (see VennDiagram) to be more certain.
T stands for "thirst". The absenceof thirst does NOT indicate the absence of dehydration. However, the presenceof thirst IS an indication of dehydration and the need to drink. Therefore, ifthirst is present, combine that with urine or body weight information (see VennDiagram) to be more certain.
|
SIMPLE TESTS TO DETERMINE IF YOU ARE DEHYDRATED
There arethree simple questions you can ask yourself to determine if you are dehydrated:
- Am I thirsty?
- Is my morningurine dark yellow?
- Is my bodyweight this morning noticeably lower when compared to yesterday morning?
If theanswer to any one of these questions is "Yes," you may be dehydrated. If theanswer to any two of these questions is "Yes," it is likely that you aredehydrated. If the answer to all three of these questions is "Yes," it is verylikely that you are dehydrated.
Drinkingtoo little or too much during exercise can be dangerous to your health and canworsen your performance. Here are some tips to help you stay in fluid balance.
- To determine howmuch fluid you lose or gain during training or competition, use a chart likethe one below to record your nude body weight to the nearest pound before andafter your workouts.
- If you lost morethan 1% of your body weight, you drank too little during exercise; if yougained weight, you drank too much.
- If you regularlylose more than 1% of your body weight, try to drink more during and after exerciseto keep your body weight stable.
- Remember, it canbe dangerous to gain weight during exercise by drinking too much.
|
RECORD OF BODY WEIGHT, THIRST, AND URINE COLOR Loss of >1% body weight or persistent thirst or dark urine indicates possible dehydration. |
||||||
|
Date |
Nude Weight Yesterday Morning |
Nude Weight this Morning |
Weight Change |
Thirsty? |
Dark Yellow Urine in Morning? |
Your Comments |
|
Example 1/1/2006 |
146 |
142 |
-4 |
Yes |
Yes |
- Very likely dehydrated - Need to drink more during and after exercise |








